Summary
Definition
History and exam
Key diagnostic factors
- abdominal pain
- nausea and vomiting
- anorexia
- signs of hypovolemia
Other diagnostic factors
- signs of organ dysfunction
- Grey-Turner sign
- Cullen sign
- Fox sign
- abdominal distention
Risk factors
- middle-aged women
- young- to middle-aged men
- gallstones
- alcohol
- hypertriglyceridemia
- hypercalcemia
- use of causative drugs
- mumps
- coxsackievirus
- Mycoplasma pneumoniae
- endoscopic retrograde cholangiopancreatography (ERCP)
- trauma
- pancreas divisum
- pancreatic cancer
- sphincter of Oddi dysfunction
- family history of pancreatitis
Diagnostic tests
1st tests to order
- serum lipase (or amylase if lipase is unavailable)
- liver function tests
- CBC and differential
- hematocrit
- BUN and serum electrolytes
- arterial blood gas
- CRP
- transabdominal ultrasound
- chest x-ray
- ratio of serum lipase:amylase
- serum triglycerides
Tests to consider
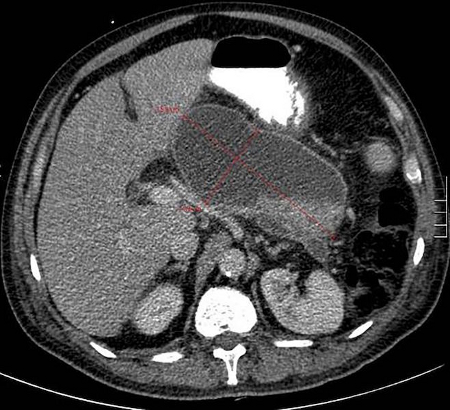
- abdominal CT scan
- magnetic resonance imaging/magnetic resonance cholangiopancreatography (MRI/MRCP)
- endoscopic ultrasound (EUS)
Emerging tests
- procalcitonin
Treatment algorithm
all patients
deteriorating or failing to improve
Contributors
Expert advisers
Scott Tenner, MD, MPH, JD, FACG
Clinical Professor of Medicine
Director, The Greater New York Endoscopy Surgical Center
Director, Brooklyn Gastroenterology and Endoscopy
State University of New York, NY
Disclosures
ST is an author of references cited in this topic. He declares that he has no other competing interests.
Craig T. Tenner, MD, FACP
Associate Professor
Medicine
New York University School of Medicine, NY
Disclosures
CTT declares that he has no competing interests.
Acknowledgements
Dr Scott Tenner and Dr Craig T. Tenner would like to gratefully acknowledge Dr Nicholas J. Zyromski, Dr Brian Daley, Dr Catherine Lindsay McKnight, and Dr Fernando Aycinena, previous contributors to this topic. They would also like to thank Dr Camille Blackledge for her contribution to this topic.
Disclosures
NJZ is an author of a reference cited in this topic. BD, CLM, FA, and CB declare that they have no competing interests.
Peer reviewers
Tamas A. Gonda, MD
Assistant Professor of Medicine
Attending Physician and Director of Research
Columbia University Medical Center
New York, NY
Disclosures
TAG declares that he has no competing interests.
Alan Moss, MD
Harvard Medical Faculty Physician
Division of Gastroenterology
Beth Israel Deaconess Medical Center
Boston, MA
Disclosures
AM declares that he has no competing interests.
Derek O'Reilly, MD
Consultant Hepatobiliary & Pancreatic Surgeon
Department of Surgery
North Manchester General Hospital
Manchester
UK
Disclosures
DOR is an author of a reference cited in this topic. He declares that he has no other competing interests.
Eric Frykberg, MD
Professor
Department of Surgery
Division General Surgery
Shands Jacksonville Medical Center, FL
Disclosures
At the time of the peer review, Dr E. Frykberg declared no competing interests. We were made aware that Dr Frykberg is now deceased.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Tenner S, Vege S, Sheth S, et al. American College of Gastroenterology guidelines: management of acute pancreatitis. Am J Gastroenterol. 2024 Mar 119(3):419-37.Full text Abstract
Leppäniemi A, Tolonen M, Tarasconi A, et al. 2019 WSES guidelines for the management of severe acute pancreatitis. World J Emerg Surg. 2019 Jun 13;14:27.Full text Abstract
Working Group IAP/APA Acute Pancreatitis Guidelines. IAP/APA evidence-based guidelines for the management of acute pancreatitis. Pancreatology. 2013 Jul-Aug;13(4 Suppl 2):e1-15.Full text Abstract
American College of Radiology. ACR appropriateness criteria: acute pancreatitis. 2019 [internet publication].Full text
Crockett SD, Wani S, Gardner TB, et al. American Gastroenterological Association Institute guideline on initial management of acute pancreatitis. Gastroenterology. 2018 Mar;154(4):1096-101.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Peptic ulcer disease
- Perforated viscus
- Esophageal spasm
More DifferentialsGuidelines
- American College of Gastroenterology guidelines: management of acute pancreatitis
- American College of Gastroenterology guidelines: management of acute pancreatitis
More GuidelinesVideos
Venepuncture and phlebotomy: animated demonstration
Radial artery puncture animated demonstration
More videosPatient information
Pancreatitis, acute
Pancreatic cancer
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer