Summary
Definition
History and exam
Key diagnostic factors
- irregular pulse rate
Other diagnostic factors
- palpitations
- hypotension
- elevated jugular venous pressure
- added heart sounds
- dizziness
- dyspnea
- rales
- evidence of stroke
Risk factors
- increasing age
- hypertension
- orthostatic hypotension
- diabetes mellitus
- heart failure
- valvular and structural heart disease
- coronary artery disease and acute coronary syndromes
- other atrial arrhythmias
- sepsis and critical illness
- cardiac or thoracic surgery
- obesity
- hyperthyroidism
- hypoxic pulmonary conditions
- alcohol consumption
- smoking
- inflammatory disorders
- excessive exercise
- height
- cancer and chemotherapy
Diagnostic tests
1st tests to order
- ECG
- serum electrolytes
- cardiac biomarkers
- thyroid function tests
- CXR
- transthoracic echocardiogram
- transesophageal echocardiogram (TEE)
Tests to avoid
- coronary CT angiography
Tests to consider
- electrophysiologic study
- exercise stress tests
Treatment algorithm
hemodynamically unstable
hemodynamically stable with left atrial thrombus, or presence of thrombus unknown/duration of AF unknown
hemodynamically stable without left atrial thrombus: symptom onset <48 hours
hemodynamically stable without left atrial thrombus: symptom onset ≥48 hours
hemodynamically stable without left atrial thrombus: asymptomatic
Contributors
Expert advisers
Arti N. Shah, MS, MD
Director
Cardiac Electrophysiology
Elmhurst Hospital Center
Elmhurst
Assistant Professor of Medicine
Mount Sinai School of Medicine
New York, NY
Disclosures
ANS declares that she has no competing interests.
Bharat K. Kantharia, MD, FRCP, FAHA, FACC, FESC, FHRS
Clinical Professor of Medicine
Icahn School of Medicine at Mount Sinai
President
Cardiovascular and Heart Rhythm Consultants
Attending and Consultant Cardiac Electrophysiologist
Mount Sinai Hospitals
New York Methodist Hospital
New York, NY
Disclosures
BKK declares that he has no competing interests.
Peer reviewers
Diwakar Jain, MD, FACC, FRCP, FASNC
Professor of Medicine (Cardiology)
Westchester Medical Center
Valhalla, NY
Disclosures
DJ declares that he has no competing interests.
Farooq A. Padder, MD, MRCP, FACC
Assistant Professor of Medicine
Hahnemann University Hospital
Woodbury, NJ
Disclosures
FAP declares that he has no competing interests.
Kim Rajappan, MA, MD, MRCP
Consultant Cardiologist and Electrophysiologist
Cardiac Department
John Radcliffe Hospital
Oxford
UK
Disclosures
KR declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Joglar JA, Chung MK, Armbruster AL, et al. 2023 ACC/AHA/ACCP/HRS guideline for the diagnosis and management of atrial fibrillation: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines. Circulation. 2024 Jan 2;149(1):e1-156.Full text Abstract
Van Gelder IC, Rienstra M, Bunting KV, et al. 2024 ESC guidelines for the management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J. 2024 Sep 29;45:3314-414.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
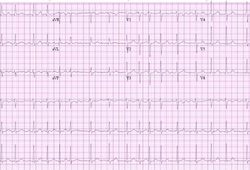
Differentials
- Atrial flutter
- Wolff-Parkinson-White syndrome
- Atrial tachycardia
More DifferentialsGuidelines
- 2024 ESC guidelines for the management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS)
- 2023 ACC/AHA/ACCP/HRS guideline for the diagnosis and management of atrial fibrillation: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines
More GuidelinesCalculators
GARFIELD-AF
Atrial Fibrillation CHA(2)DS(2)-VASc Score for Stroke Risk
More CalculatorsVideos
How to perform an ECG: animated demonstration
More videosPatient information
Atrial fibrillation: what is it?
Atrial fibrillation: what treatments work?
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer