Summary
Definition
History and exam
Key diagnostic factors
- age 20 to 34 years
- testicular mass
Other diagnostic factors
- extratesticular manifestation
Risk factors
- cryptorchidism
- gonadal dysgenesis
- family history of testicular cancer
- personal history of testicular cancer
- testicular atrophy
- white ethnicity
- HIV infection
- occupational exposures
- inguinal hernia
- genetic abnormality
Diagnostic tests
1st tests to order
- ultrasound with color Doppler of testis
- chest imaging
- CT scan abdomen and pelvis with contrast
- serum beta-human chorionic gonadotropin (beta-hCG)
- serum alpha-fetoprotein (AFP)
- serum LDH
- histologic exam of testicular mass postorchiectomy
Tests to consider
- MRI abdomen and pelvis
- MRI brain
- CT scan chest
- biopsy of contralateral testis
Emerging tests
- microRNA
Treatment algorithm
suspicious testicular mass
early-stage seminoma
early-stage nonseminoma
seminoma or nonseminoma: stage IIC or stage III disease
seminoma or nonseminoma: relapsed disease
Contributors
Authors
Al B. Barqawi, MD, FRCS
Professor of Surgery/Urology
University of Colorado Anschutz Medical Campus
Aurora
CO
Disclosures
ABB declares that he has no competing interests.
Corbin J. Eule, MD
Assistant Professor of Medical Oncology
University of Colorado Anschutz Medical Campus
Aurora
CO
Disclosures
CJE declares that he has no competing interests.
Acknowledgements
Dr Al B. Barqawi and Dr Corbin J. Eule would like to gratefully acknowledge Dr Elizabeth R. Kessler, Dr Thomas W. Flaig, and Dr Brandon Bernard, previous contributors to this topic.
Disclosures
ERK, TWF, and BB declare that they have no competing interests.
Peer reviewers
Aditya Bagrodia, MD, FACS
UC San Diego Health
San Diego
CA
Disclosures
AB declares that he has no competing interests.
Gianfilippo Bertelli, MD, PhD, FRCP (Edin)
Consultant/Honorary Senior Lecturer in Medical Oncology
SW Wales Cancer Institute/Department of Oncology
Singleton Hospital
Sketty
Swansea
UK
Disclosures
GB declares that he has no competing interests.
Emilio Porfiri, MD, PhD
Senior Lecturer in Medical Oncology
School of Cancer Sciences
University of Birmingham
Birmingham
UK
Disclosures
EP declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Stephenson A, Bass EB, Bixler BR, et al. Diagnosis and treatment of early-stage testicular cancer: AUA guideline amendment 2023. J Urol. 2024 Jan;211(1):20-5.Full text Abstract
European Association of Urology. Testicular cancer. 2025 [internet publication].Full text
Oldenburg J, Berney DM, Bokemeyer C, et al. Testicular seminoma and non-seminoma: ESMO-EURACAN clinical practice guideline for diagnosis, treatment and follow-up. Ann Oncol. 2022 Apr;33(4):362-75.Full text Abstract
National Comprehensive Cancer Network. NCCN clinical practice guidelines in oncology: testicular cancer [internet publication].Full text
American College of Radiology. ACR appropriateness criteria: staging and surveillance of testicular cancer. 2021 [internet publication].Full text
Gillessen S, Sauvé N, Collette L, et al. Predicting outcomes in men with metastatic nonseminomatous germ cell tumors (NSGCT): results from the IGCCCG update consortium. J Clin Oncol. 2021 May 10;39(14):1563-74.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
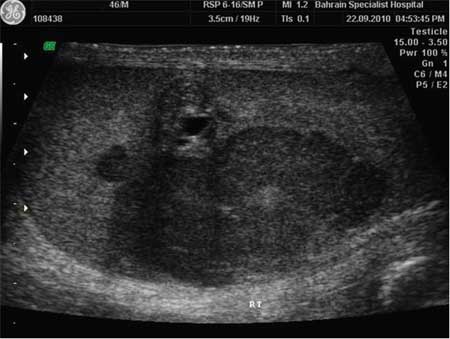
Differentials
- Testicular torsion
- Epididymo-orchitis
- Scrotal hernia
More DifferentialsGuidelines
- Guidelines on testicular cancer
- Diagnosis and treatment of early stage testicular cancer
More GuidelinesPatient information
Testicular cancer
Testicular cancer: questions to ask your doctor
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer