Summary
Definition
History and exam
Key diagnostic factors
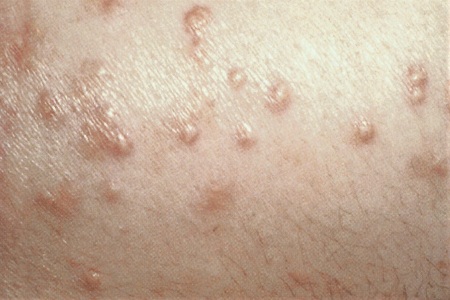
- eruptive xanthomas
- lipemia retinalis
Other diagnostic factors
- increased BMI/waist circumference
- lipodystrophy
- features of coronary artery disease
- claudication
- neurologic features
- recurrent abdominal pain
Risk factors
- family history of hyperlipidemia
- high saturated fat diet
- high carbohydrate or high glycemic index diet
- excessive alcohol consumption
- family or personal history of overweight/obesity
- family or personal history of diabetes
- insulin resistance
- liver disease
- renal disease
- HIV infection
- use of certain drugs
- Cushing syndrome
- inflammatory/immune disorders
- organ transplant
- hypothyroidism
- pregnancy
Diagnostic tests
1st tests to order
- triglyceride level
Tests to consider
- apolipoprotein B
- fasting plasma glucose
- BUN, creatinine
- urinary albumin/protein
- serum albumin
- thyroid-stimulating hormone
- liver function tests
- C-reactive protein
Treatment algorithm
chylomicronemia
moderate HTG (fasting TG ≥150 mg/dL [≥1.7 mmol/L] or nonfasting TG ≥175 mg/dL [≥2.0 mmol/L] and TG <500 mg/dL [<5.6 mmol/L])
severe HTG (fasting TG ≥500 mg/dL [≥5.6 mmol/L] especially fasting TG ≥1000 mg/dL [≥11.3 mmol/L])
Contributors
Authors
Robert A. Hegele, MD, FRCPC, Cert Endo, FACP, FAHA
Jacob J. Wolfe Distinguished Medical Research Chair
Martha Blackburn Chair in Cardiovascular Research
Distinguished University Professor of Medicine and Biochemistry
University of Western Ontario
London
Ontario
Canada
Disclosures
RAH reports consulting fees from Akcea/Ionis, Amgen, HLS Therapeutics, Medison, Novartis, Pfizer, Regeneron, Sanofi and Ultragenyx. RAH is an author of references cited in this topic.
Acknowledgements
Dr Robert A. Hegele would like to gratefully acknowledge Dr David Alexander Leaf, the previous contributor to this topic.
Disclosures
DAL declares that he has no competing interests.
Peer reviewers
Vinaya Simha, MBBS, MD
Associate Professor
Mayo Clinic
Rochester
MN
Disclosures
VS declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. Circulation. 2019 Jun 18;139(25):e1082-143.Full text Abstract
Mach F, Baigent C, Catapano AL, et al. 2019 ESC/EAS guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur Heart J. 2020 Jan 1;41(1):111-88.Full text Abstract
Patel SB, Wyne KL, Afreen S, et al. American Association of Clinical Endocrinology clinical practice guideline on pharmacologic management of adults with dyslipidemia. Endocr Pract. 2025 Feb;31(2):236-62.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Diabetes
- Lipodystrophies
- Liver disease
More DifferentialsGuidelines
- 2025 AACE clinical practice guidelines on the pharmacologic management of adults with dyslipidemia
- 2025 focused update of the 2019 ESC/EAS guidelines for the management of dyslipidaemias
More GuidelinesPatient information
High cholesterol
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer