Summary
Definition
History and exam
Other diagnostic factors
- sore throat
- neck lump
- indurated or ulcerated mass
- dysphagia
- oral pain
- weight loss
- otalgia
- trismus
- white plaques (leukoplakia) and red plaques (erythroplakia)
Risk factors
- human papillomavirus (HPV) infection
- smoking tobacco cigarettes
- alcohol
- tobacco and betel nut chewing
Diagnostic tests
1st tests to order
- biopsy of the primary site
- CT scan of the head and neck
- fine needle aspiration cytology (FNAC) of neck nodes
- in situ hybridization for human papillomavirus (HPV)-16, p16 immunohistochemistry, or PCR in biopsy specimen
Tests to consider
- MRI of the head and neck
- PET-CT of the head and neck
- panendoscopy or triple endoscopy
- modified barium swallow
- excision biopsy of neck nodes
- circulating tumor high-risk HPV DNA
- CBC
- electrolytes
- BUN
- serum creatinine
- total protein
- albumin
- prealbumin
- LFTs
Treatment algorithm
Human papillomavirus (HPV)-negative
HPV-positive
recurrent disease
Contributors
Authors
Linda X. Yin, MD
Assistant Professor
Department of Otolaryngology - Head & Neck Surgery
Mayo Clinic Rochester
Rochester
MN
Disclosures
LXY declares that she has no competing interests.
Melina J. Windon, MD
Assistant Professor
Department of Otolaryngology - Head & Neck Surgery
University of Kentucky
Lexington
KY
Disclosures
MJW declares that she has no competing interests.
Acknowledgements
Dr Linda X. Yin and Dr Melina J. Windon would like to gratefully acknowledge Dr Anuraag Parikh, Dr Nam P. Nguyen, Dr Fabio Almeida, and Dr Linda Garland, previous contributors to this topic.
Disclosures
AP declares that he has no competing interests. AP's spouse is an employee of and holds stock in Regeneron Pharmaceuticals. LG is on the speakers' bureau for Sanofi-Aventis, maker of Taxotere. NPN is an author of a number of references cited in this topic. FA declares that he has no competing interests.
Peer reviewers
AJ Balm, MD, PhD, FACS, FRCS
Chair Emeritus
Head and Neck Multidisciplinary Cooperative Group
Department of Head & Neck Oncology and Surgery
The Netherlands Cancer Institute
Amsterdam
The Netherlands
Disclosures
AJB declares that he has no competing interests.
Andy Trotti, MD
Specializing in Head & Neck Cancer
Director of Clinical Trials
Radiation Oncology
H. Lee Moffitt Cancer Center & Research Institute
Tampa
FL
Disclosures
AT is an author of a reference cited in this topic.
Hari Deshpande, MD
Assistant Professor of Medicine
Yale Cancer Center
Yale University
New Haven
CT
Disclosures
HD is on the speakers' bureau for Sanofi-Aventis and has received reimbursement for talks given about their product Taxotere.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
National Comprehensive Cancer Network. NCCN clinical practice guidelines in oncology: head and neck cancers [internet publication].Full text
Amin MB, Edge SB, Greene FL, et al, eds. AJCC cancer staging manual. 8th ed. New York, NY: Springer International Publishing, 2017.
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
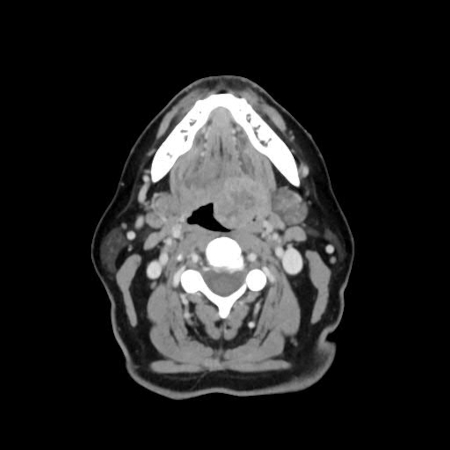
Differentials
- Tonsillitis
- Aphthous ulcer
- Oral syphilis
More DifferentialsGuidelines
- NCCN clinical practice guidelines in oncology: head and neck cancers
- Prevention and management of osteoradionecrosis in patients with head and neck cancer treated with radiation therapy
More GuidelinesPatient information
Quitting smoking
Sore throat
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer