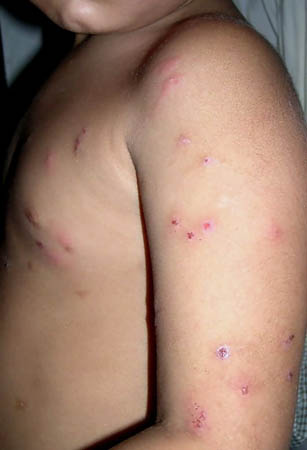
Summary
Definition
History and exam
Key diagnostic factors
- acute to subacute recurrent skin eruption
- polymorphic, generalized, nonpruritic skin eruption
Other diagnostic factors
- scars or pigment changes
- immunosuppression
- recent illness
- family history of pityriasis lichenoides
- headache
- myalgias/arthralgias
- malaise
- burning/pruritus
- multiorgan failure
Risk factors
- childhood to early adult age
- male sex
- HIV
Diagnostic tests
1st tests to order
- dermoscopy
- skin biopsy
Tests to consider
- antistreptolysin titers
- Epstein-Barr virus IgM/IgG viral capsid antigen and nuclear antigen antibody
- monospot or heterophil antibody test
- hepatitis B surface antigen, antisurface antibody, and anticore IgM
- hepatitis C virus antibody
- HIV screening
- rapid plasma reagin
- throat cultures
- toxoplasma Sabin-Feldman dye test, indirect immunofluorescence/hemagglutination
- erythrocyte sedimentation rate
- CRP
- serum LDH
- WBC count
- serum albumin
Treatment algorithm
mild to moderate disease
severe disease or treatment resistance
Contributors
Authors
Amy Musiek, MD
Professor of Dermatology
Division of Dermatology
Washington University School of Medicine in St. Louis
St. Louis
MO
Disclosures
AM is a paid lecturer in cutaneous T-cell lymphoma for Dermatology Week, is the author of the UpToDate article on Pityriasis lichenoides chronica, and is an investigator for multiple industry sponsored studies all unrelated to pityriasis lichenoides.
Acknowledgements
Dr Amy Musiek would like to gratefully acknowledge Dr Amer Khachemoune and Dr Marianna Blyumin-Karasik, previous contributors to this topic.
Disclosures
AK and MB-K declare that they have no competing interests.
Peer reviewers
Andrew D. Lee, MD
Resident
Department of Dermatology
Wake Forest University School of Medicine
Winston-Salem
NC
Disclosures
ADL declares that he has no competing interests.
Abdulhafez Selim, MD
Assistant Professor
King Fahd University of Petroleum and Minerals
Dhahran
Saudi Arabia
Disclosures
AS declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Khachemoune A, Blyumin ML. Pityriasis lichenoides: pathophysiology, classification, and treatment review. Am J Clin Dermatol. 2007;8(1):29-36. Abstract
Bowers S, Warshaw EM. Pityriasis lichenoides and its subtypes. J Am Acad Dermatol. 2006 Oct;55(4):557-72; quiz 573-6. Abstract
Bellinato F, Maurelli M, Gisondi P, et al. A systematic review of treatments for pityriasis lichenoides. J Eur Acad Dermatol Venereol. 2019 Nov;33(11):2039-49. Abstract
Jung F, Sibbald C, Bohdanowicz M, et al. Systematic review of the efficacies and adverse effects of treatments for pityriasis lichenoides. Br J Dermatol. 2020 Dec;183(6):1026-32. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
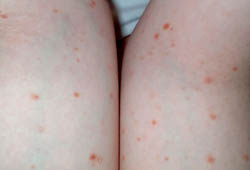
Differentials
- Lymphomatoid papulosis
- Guttate psoriasis
- Drug eruption
More DifferentialsPatient information
Psoriasis: what is it?
Psoriasis: what are the treatment options?
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer