Resumo
Definição
História e exame físico
Principais fatores diagnósticos
- active symmetric arthritis lasting >6 weeks
- age 50 to 55 years
- female sex
- joint pain
- joint swelling
Outros fatores diagnósticos
- morning stiffness
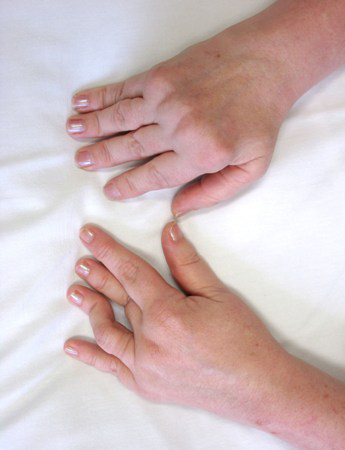
- swan neck deformity
- Boutonniere deformity
- ulnar deviation
- rheumatoid nodules
- vasculitic lesions
- pleuritic chest pain
- scleritis and/or uveitis
Fatores de risco
- genetic predisposition
- smoking
- overweight or obesity
- infection
Investigações diagnósticas
Primeiras investigações a serem solicitadas
- rheumatoid factor (RF)
- anticyclic citrullinated peptide (anti-CCP) antibody
- radiographs
- ultrasonography
Investigações a serem consideradas
- disease activity score(s)
- MRI
Algoritmo de tratamento
mild disease activity at initial presentation: not pregnant or planning pregnancy
moderate-to-severe disease activity at initial presentation: not pregnant or planning pregnancy
pregnant or planning pregnancy
failure to reach low disease activity after 3 months of therapy: not pregnant or planning pregnancy
Colaboradores
Autores
Yusuf Yazici, MD

Clinical Associate Professor of Medicine
New York University School of Medicine
New York
NY
Declarações
YY receives research support from BMS and Amgen; he has consulted for Amgen, BMS, Hemay, Chugai, and Sanofi.
Revisores
Joshua F. Baker, MD, MSCE
Associate Professor of Medicine and Epidemiology
University of Pennsylvania
Pennsylvania
PA
Declarações
JFB has received consulting fees from Bristol-Myers Squibb, Pfizer, Cumberland Pharma, and CorEvitas.
Créditos aos pareceristas
Os tópicos do BMJ Best Practice são constantemente atualizados, seguindo os desenvolvimentos das evidências e das diretrizes. Os pareceristas aqui listados revisaram o conteúdo pelo menos uma vez durante a história do tópico.
Declarações
As afiliações e declarações dos pareceristas referem--se ao momento da revisão.
Referências
Principais artigos
Fraenkel L, Bathon JM, England BR, et al. 2021 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2021 Jul;73(7):1108-23.Texto completo Resumo
National Institute for Health and Care Excellence. Rheumatoid arthritis in adults: management. Oct 2020 [internet publication].Texto completo
Smolen JS, Landewé RBM, Bergstra SA, eta al. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2022 update. Ann Rheum Dis. 2023 Jan;82(1):3-18 Epub 2022 Nov 10.Texto completo Resumo
Artigos de referência
Uma lista completa das fontes referenciadas neste tópico está disponível para os usuários com acesso total ao BMJ Best Practice.
Diagnósticos diferenciais
- Psoriatic arthritis (PsA)
- Infectious arthritis
- Gout
Mais Diagnósticos diferenciaisDiretrizes
- 2023 American College of Rheumatology (ACR) guideline for the screening and monitoring of interstitial lung disease in people with systemic autoimmune rheumatic disease
- Guideline for vaccinations in patients with rheumatic and musculoskeletal diseases
Mais DiretrizesFolhetos informativos para os pacientes
Rheumatoid arthritis
Rheumatoid arthritis: questions to ask your doctor
Mais Folhetos informativos para os pacientesConectar-se ou assinar para acessar todo o BMJ Best Practice
O uso deste conteúdo está sujeito ao nosso aviso legal