Summary
Definition
History and exam
Key diagnostic factors
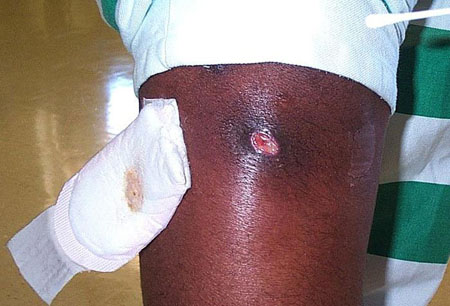
- erythematous skin lesions or pustules, in single or multiple forms
- irritation or pain at indwelling catheter site
- heart murmur and other signs of endocarditis
Other diagnostic factors
- infection unresponsive to penicillins
- history of a presumed spider bite
- abscess formation
- fever
- fatigue
- tachycardia and hypotension
- shortness of breath and cough
- painful urination, hematuria, or urinary retention
- night sweats or chills
- altered mental status
- signs of pulmonary consolidation
- abdominal pain or flank pain
- joint pain
- joint swelling
Risk factors
- age >50 years (healthcare-associated)
- children and younger adults <35 years (community-associated)
- men who have sex with men (community-associated)
- intravenous drug users (community-associated)
- indwelling device or current wound (healthcare-associated)
- hospitalization within the last year (healthcare-associated)
- chronic illness requiring healthcare visits (healthcare-associated)
- crowded conditions/semi-closed communities (healthcare-associated and community-associated)
- previous history of MRSA (healthcare-associated and community-associated)
- exposure to an MRSA-positive person (healthcare-associated and community-associated)
- nasal colonization with MRSA (healthcare-associated and community-associated)
- prior antibiotic use (healthcare-associated and community-associated)
- HIV infection (community-associated and healthcare-associated)
Diagnostic tests
1st tests to order
- CBC
- blood culture
- urine culture
- tissue culture
- sputum culture
- echocardiogram
- CXR
- arthrocentesis fluid culture
- indwelling vascular catheter tip culture
Tests to consider
- polymerase chain reaction (PCR)
Treatment algorithm
skin and soft-tissue infection: community-associated
skin and soft-tissue infection: healthcare-associated
bacteremia
pneumonia
visceral abscess
endocarditis
septic arthritis
urinary tract infection (UTI)
osteomyelitis
recurrent skin and soft-tissue MRSA infections in colonized patients
Contributors
Authors
Kyle J. Popovich, MD MS
Professor of Medicine
Rush University Medical Centre
Chicago
IL
Disclosures
KJP declares that she has no competing interests.
Acknowledgements
Dr Kyle J. Popovich would like to gratefully acknowledge Dr Dara Grennan, Dr Paul F. Roberts, and Dr R. John Presutti, the previous contributors to this topic.
Disclosures
DG, PFR, and RJP declare that they have no competing interests.
Peer reviewers
Chad M. Hivnor, Major, USAF, MC, FS
Chief
Outpatient & Pediatric Dermatology
59th Medical Wing/ SGOMD
Lackland Air Force Base
San Antonio
TX
Disclosures
CMH declares that he has no competing interests.
Linda Kalilani, MBBS, MPhil, PhD
Epidemiologist
College of Medicine
University of Malawi
Zomba
Malawi
Disclosures
LK declares that she has no competing interests.
Christine Radojicic, MD
Professor
Cleveland Clinic Foundation
Cleveland
OH
Disclosures
CR declares that she has no competing interests.
Alistair Leanord, BSc, MBChB, MD, DTM&H, FRCPath
Consultant Microbiologist
Microbiology Department
Southern General Hospital
Glasgow
UK
Disclosures
AL declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Gorwitz RJ. A review of community-associated methicillin-resistant Staphylococcus aureus skin and soft tissue infections. Pediatr Infect Dis J. 2008 Jan;27(1):1-7. Abstract
Nathwani D, Morgan M, Masterton RG, et al. Guidelines for UK practice for the diagnosis and management of methicillin-resistant Staphylococcus aureus (MRSA) infections presenting in the community. J Antimicrob Chemother. 2008 May;61(5):976-94.Full text Abstract
Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis. 2014 Jul 15;59(2):e10-52.Full text Abstract
Brown NM, Goodman AL, Horner C, et al. Treatment of methicillin-resistant Staphylococcus aureus (MRSA): updated guidelines from the UK. JAC Antimicrob Resist. 2021 Mar;3(1):dlaa114.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Insect or spider bite
- Cellulitis
- Folliculitis
More DifferentialsGuidelines
- Practice recommendation: strategies to prevent methicillin-resistant Staphylococcus aureus transmission and infection in acute-care hospitals: 2022 update
- Strategies to prevent surgical site infections in acute-care hospitals: 2022 update
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer