Summary
Definition
History and exam
Key diagnostic factors
- colicky abdominal pain
- abdominal distention
- nausea
- vomiting
- change in bowel habits
- hard feces
- soft stools
- empty rectum
- recent weight loss
- rectal bleeding
- palpable rectal mass
- palpable abdominal mass
- tympanic abdomen
- abnormal bowel sounds
- fever
- abdominal tenderness
- abdominal rigidity
Other diagnostic factors
- tenesmus
Risk factors
- colorectal cancer
- current or previous malignancy
- diverticular disease
- colonic volvulus
- inflammatory bowel disease
- current or previous hernia
- endometriosis
- diabetes
- previous abdominal surgery
- megacolon
- low or high dietary fiber
- laxative abuse
- previous radiation therapy
- ingestion of foreign body
Pruebas diagnósticas
Primeras pruebas diagnósticas para solicitar
- CT abdomen and pelvis
- CBC
- serum electrolytes
- CRP
- renal function
- glucose
- coagulation studies, type and screen, cross-match
- blood gas analysis (including lactate)
- serum amylase/lipase
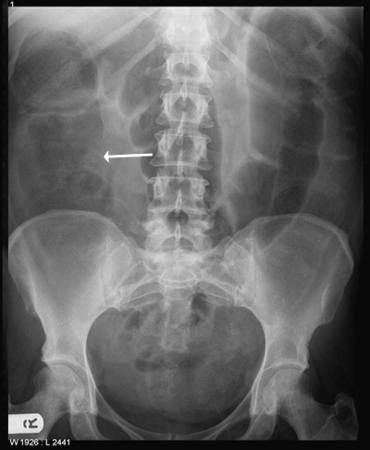
- plain abdominal x-ray
Pruebas diagnósticas que deben considerarse
- beta-human chorionic gonadotrophin
- urinalysis
- abdominal ultrasound
- contrast enema
- flexible/rigid endoscopy
- biopsy
Algoritmo de tratamiento
acutely ill
sigmoid volvulus
cecal volvulus
colorectal malignancy
diverticular disease
foreign body ingestion
benign strictures
pelvic abscess
currently receiving palliative care
Colaboradores
Consejeros especializados
Adrian Maung, MD, MBA, FACS, FCCM
Associate Professor of Surgery
Division of General Surgery, Trauma and Surgical Critical Care
Department of Surgery
Yale School of Medicine
New Haven, CT
Divulgaciones
AM declares that he has no competing interests.
Agradecimientos
Dr Adrian A. Maung would like to gratefully acknowledge Dr George Malietzis, Dr John T. Jenkins, and Dr Alisdair J. MacDonald, previous contributors to this topic.
Divulgaciones
GM, JTJ, and AJM declare that they have no competing interests.
Revisores por pares
Alessandro Fichera, MD, FACS, FASCRS
Assistant Professor
Department of Surgery
University of Chicago
Chicago, IL
Divulgaciones
AF declares that he has no competing interests.
Robert H. Diament, MD
Consultant Surgeon
Crosshouse Hospital
Crosshouse
Kilmarnock
UK
Divulgaciones
RHD declares that he has no competing interests.
Agradecimiento de los revisores por pares
Los temas de BMJ Best Practice se actualizan de forma continua de acuerdo con los desarrollos en la evidencia y en las guías. Los revisores por pares listados aquí han revisado el contenido al menos una vez durante la historia del tema.
Divulgaciones
Las afiliaciones y divulgaciones de los revisores por pares se refieren al momento de la revisión.
Referencias
Artículos principales
Alavi K, Poylin V, Davids JS, et al. The American Society of Colon and Rectal Surgeons clinical practice guidelines for the management of colonic volvulus and acute colonic pseudo-obstruction. Dis Colon Rectum. 2021 Sep 1;64(9):1046-57.Texto completo Resumen
Pisano M, Zorcolo L, Merli C, et al. 2017 WSES guidelines on colon and rectal cancer emergencies: obstruction and perforation. World J Emerg Surg. 2018 Aug 13;13:36.Texto completo Resumen
Naveed M, Jamil LH, Fujii-Lau LL, et al. American Society for Gastrointestinal Endoscopy guideline on the role of endoscopy in the management of acute colonic pseudo-obstruction and colonic volvulus. Gastrointest Endosc. 2020 Feb;91(2):228-35. Resumen
Artículos de referencia
Una lista completa de las fuentes a las que se hace referencia en este tema está disponible para los usuarios con acceso a todo BMJ Best Practice.
Diferenciales
- Acute colonic pseudo-obstruction (Ogilvie syndrome)
- Chronic/idiopathic megacolon
- Toxic megacolon
Más DiferencialesGuías de práctica clínica
- WSES consensus guidelines on sigmoid volvulus management
- 2017 WSES guidelines on colon and rectal cancer emergencies: obstruction and perforation
Más Guías de práctica clínicaVideos
Venepuncture and phlebotomy: animated demonstration
Central venous catheter insertion: animated demonstration
Más vídeosFolletos para el paciente
Bowel cancer
Bowel cancer: questions to ask your doctor
Más Folletos para el pacienteInicie sesión o suscríbase para acceder a todo el BMJ Best Practice
El uso de este contenido está sujeto a nuestra cláusula de exención de responsabilidad