რეკომენდაციები
ძირითადი რეკომენდაციები
AKI is diagnosed by an acutely rising blood urea nitrogen (BUN) and creatinine, or sustained oliguria, in line with validated criteria such as the Kidney Disease: Improving Global Outcomes (KDIGO) definition.[1][3] The KDIGO criteria merge features of the RIFLE (Risk, Injury, Failure, Loss of kidney function, and Endstage kidney disease) and Acute Kidney Injury Network (AKIN) criteria into a single standardized definition.[4][88][89]
AKI is diagnosed if any of the following criteria are met:[1]
Increase in serum creatinine by ≥0.3 mg/dL within 48 hours, or
Increase in serum creatinine to ≥1.5 times baseline, which is known or presumed to have occurred within the prior 7 days, or
Urine volume <0.5 mL/kg/hour for 6 hours.
AKI should then be staged according to severity criteria using KDIGO, RIFLE, or AKIN classifications.[1][88][89]
The condition is often asymptomatic and only diagnosed by laboratory tests.[90] General symptoms may include nausea and vomiting. Uremia, including altered mental status, may occur but this is more commonly seen in advanced AKI or in advanced chronic kidney disease.
A history of trauma or predisposing disease (e.g., congestive heart failure, chronic kidney disease, diabetes, peripheral vascular disease, and connective tissue diseases such as systemic lupus erythematosus, scleroderma, and vasculitis) may be present. Several groups have published risk scores for AKI and these have been variably validated by follow-up studies.[50][55][91][92]
History in prerenal failure
Patients may have a history of excessive fluid loss from hemorrhage, the gastrointestinal (GI) tract (vomiting, diarrhea), or sweating. Hospitalized patients may have insufficient replacement fluids to cover ongoing and insensible losses, especially if there is restriction of enteral input.
There may be a history of sepsis, burns, major surgery, or pancreatitis.[90][93]
Patients may present with symptoms of hypovolemia: thirst, dizziness, tachycardia, oliguria, or anuria. Orthopnea and paroxysmal nocturnal dyspnea may occur if advanced cardiac failure is present.
History in intrinsic renal disease
Typically, patients present with acute tubular necrosis (ATN) subsequent to severe infection, nephrotoxic drug exposure, or major surgery. The patient may have a history of rash, hematuria, or edema with hypertension suggesting nephritic syndrome and an acute glomerulonephritis or renal vasculitis. There might have been a recent vascular intervention preceding the AKI, leading to cholesterol emboli or contrast-induced injury. A history of myeloproliferative disorder such as multiple myeloma may predispose to AKI, particularly in volume-depleted patients.
A history of all current drugs and any recent radiologic examinations should be taken to establish any exposure to potential nephrotoxins. Acyclovir, methotrexate, triamterene, indinavir, or sulfonamides can cause tubular obstruction by forming crystals. Over-the-counter drugs such as nonsteroidal anti-inflammatory drugs (NSAIDs) and sympathomimetics are often overlooked, and patients should be specifically queried about their use.[94] Allergic interstitial nephritis may be suspected in patients with a history of NSAID use or recent administration of new drugs such as beta-lactam antibiotics. Other substances to consider include hallucinogens and "bath salts".[95]
Pigment-induced AKI, due to rhabdomyolysis, should be suspected in patients presenting with muscle tenderness, seizures, drug abuse or alcohol abuse, excessive exercise, or limb ischemia (e.g., from crush injury).
History in postrenal failure
Postrenal failure is more common in older men with prostatic obstruction. There is often a history of urgency, frequency, or hesitancy.
A history of malignancy, prostatism, nephrolithiasis, or previous surgery may coincide with the diagnosis of obstruction. Obstruction caused by renal calculi or papillary necrosis typically presents with flank pain and visible hematuria.
Physical exam
Hypotension, hypertension, pulmonary edema, or peripheral edema may be present. There may be asterixis or altered mental status when uremia is present.
Patients with fluid loss, sepsis, or pancreatitis may have hypotension along with other signs of circulatory collapse.[96]
Patients with glomerular disease typically present with hypertension and edema, proteinuria, and microscopic hematuria (nephritic syndrome). Severe nephrotic syndrome, with peripheral edema and relative hypotension, can also lead to AKI.[97]
The presence of rash, petechiae, or ecchymoses may suggest an underlying systemic condition such as vasculitis, thrombotic microangiopathy, or glomerulonephritis.[71]
Patients with ATN may present after hemorrhage, sepsis, drug overdose, surgery, cardiac arrest, or other conditions associated with hypotension and prolonged renal ischemia.
An underlying abdominal bruit may support renovascular disease.
The patient with prostatic obstruction may present with abdominal distension from a full bladder.
Initial tests
Initial workup should include basic metabolic profile (including BUN and creatinine), venous blood gases, complete blood count, urinalysis and culture, urine chemistries (for fractional excretion of sodium and urea), renal ultrasound (when appropriate by history or exam), chest x-ray, and ECG. Urine osmolality is rarely ordered but, if high, suggests prerenal azotemia (in the absence of contrast dyes). Urinary eosinophil counts have low sensitivity and specificity for acute interstitial nephritis, but may be elevated in patients with pyuria.[98]
Chest x-ray may reveal pulmonary edema or cardiomegaly.
ECG may demonstrate arrhythmias if hyperkalemia is present.
Bladder catheterization is recommended in all cases of AKI, if bladder outlet obstruction is suspected and cannot be quickly ruled out by ultrasound. It is diagnostic and therapeutic for bladder neck obstruction in addition to providing an assessment of residual urine and a sample for analysis.
A serum BUN to creatinine ratio ≥20:1 supports a diagnosis of prerenal azotemia, but other causes of elevated BUN must be ruled out (such as drug-induced elevations or GI bleeding).
A fractional excretion of sodium (FENa) of <1% supports prerenal azotemia but may also be seen in glomerulonephritis, hepatorenal syndrome (typically <0.2%), and some cases of obstruction and even ATN, as long as tubular function remains intact.[99][100] The FENa is calculated as follows: (urine sodium x serum creatinine)/(serum sodium x urine creatinine) x 100%.
A fractional excretion of urea of <35% supports a diagnosis of prerenal azotemia and is helpful if the patient has had diuretic exposure. The fractional excretion of urea is calculated as follows: (urine urea x serum creatinine)/(serum urea x urine creatinine) x 100%.[99]
A fluid challenge may be administered with crystalloid or colloid (but not hydroxyethyl starch solutions), and is both diagnostic and therapeutic for suspected prerenal azotemia if renal function improves rapidly.
High urine osmolality (or an elevated urine specific gravity), seen in prerenal azotemia, suggests maintenance of normal tubular function and response to antidiuretic hormone in cases of hypovolemia. Urine sodium concentration of <20 mEq/L suggests avid sodium retention and is typical of renal hypoperfusion/prerenal azotemia.[99] High urinary sodium is often seen in ATN, but is not exclusive to the diagnosis. Urine osmolality may be very high as the result of radiocontrast dyes and mannitol.
Urinary eosinophils >5% to 7% weakly supports the presence of interstitial nephritis, but is not diagnostic.[98] Some guidelines (e.g., the American Association for Clinical Chemistry) advise against routine use of urinary eosinophils in the evaluation of AKI.[99]
If there is no identified cause of AKI, a renal ultrasound is ordered at onset of workup to assist in evaluation of obstructive causes as well as in the evaluation of renal architecture and size. It is also useful for diagnosis of underlying chronic kidney disease.
Subsequent tests
A computed tomography or magnetic resonance imaging scan may be required to further evaluate cases of obstruction suggested on ultrasound (e.g., possible masses or stones).
Nuclear renal flow scans can evaluate renal perfusion and function, and may be modified using captopril to evaluate for renal artery stenosis, or with furosemide to evaluate for obstruction in cases of mild hydronephrosis, when obvious mechanical obstruction is uncertain.
Further diagnostic tests may be determined by the suspected cause of AKI, such as cystoscopy for cases of suspected ureteral stenosis or serologic evaluation (e.g., antistreptolysin O, erythrocyte sedimentation rate, antinuclear antibodies, anti-DNA, complement, anti-glomerular basement membrane antibodies, antineutrophil cytoplasmic antibodies, acute hepatitis profile, HIV test, and cryoglobulins) if the history suggests autoimmune, vasculitis, infectious, or immune complex disease, as in cases of suspected glomerulonephritis. Novel serum and urinary biomarkers have potential as useful indicators for the diagnosis of AKI and as predictors of mortality after AKI; however, further studies are needed to determine their clinical utility.[101][102][103][104][105][106][107]
A renal biopsy may be performed for further evaluation of AKI when the history, physical exam, and other studies suggest systemic disease as etiology or when the diagnosis is unclear.
Biopsies may confirm acute tubular necrosis, but are rarely done for this condition.
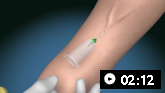
How to take a venous blood sample from the antecubital fossa using a vacuum needle.
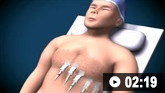
How to record an ECG. Demonstrates placement of chest and limb electrodes.
Use of this content is subject to our disclaimer