Summary
Definition
History and exam
Key diagnostic factors
- tachycardia
- tachypnea
- high (>101°F [>38°C]) or low (<96.8°F [<36°C]) temperature
- acutely altered mental status
- poor capillary refill, mottling of the skin, or ashen appearance
- signs associated with specific source of infection
- low oxygen saturation
- arterial hypotension
- decreased urine output
- cyanosis
Other diagnostic factors
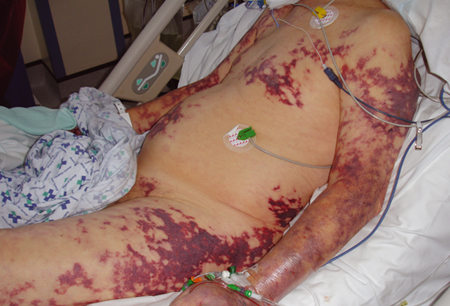
- purpura fulminans
- jaundice
- ileus
Risk factors
- age >65 years
- immunocompromised state
- indwelling intravenous lines or urinary catheters
- recent surgery or other invasive procedures
- hemodialysis
- diabetes mellitus
- intravenous drug use
- alcohol use disorder
- breached skin integrity
- pregnancy
- urban residence
- lung disease
- male sex
- non-white ancestry
- winter season
Diagnostic tests
1st tests to order
- blood culture
- lactate levels
- CBC with differential
- blood urea nitrogen (BUN) and serum electrolytes
- serum creatinine
- liver function tests
- coagulation studies (INR, activated PTT)
- serum glucose
- CRP
- other cultures (e.g., of sputum, stool, urine, wounds, catheters, prosthetic implants, epidural sites, pleural or peritoneal fluid)
- arterial blood gas (ABG) or venous blood gas (VBG)
- chest x-ray
- ECG
Tests to consider
- lumbar puncture
- echocardiogram (transthoracic or transesophageal)
- ultrasound scan
- CT chest or abdomen
- serum procalcitonin
Treatment algorithm
presumed or confirmed sepsis
Contributors
Expert advisers
Andre C. Kalil, MD, MPH, FACP, FIDSA, FCCM
Professor
Department of Internal Medicine
Division of Infectious Diseases
University of Nebraska Medical Center
Omaha, NE
Disclosures
ACK declares that he has no competing interests.
Kelly Cawcutt, MD, MS, FACP, FIDSA, FCCM
Associate Professor
Department of Internal Medicine
Division of Pulmonary, Critical Care, Sleep & Allergy
University of Nebraska Medical Center
Omaha, NE
Disclosures
KC has received payment for medical writing from IDSA and CloroxPro. KC has received honoraria for creation of educational materials from the Society for Healthcare Epidemiology of America (SHEA) and payment from BD. KC has received honoraria and travel expenses from NAPA. KC has received payment for book proposal review from Elsevier. KC has participated as author, lecturer, and committee member for the Society of Critical Care Medicine (SCCM) course and book, providing content on controversies in sepsis.
Acknowledgements
Professor Andre Kalil and Dr Kelly Cawcutt would like to gratefully acknowledge Dr Ron Daniels, Dr Matt Inada-Kim, Dr Aamir Saifuddin, Dr Tim Nutbeam, Dr Edward Berry, Dr Lewys Richmond, and Dr Paul Kempen, previous contributors to this topic.
Disclosures
RD has received payment for consultancy on sepsis from Kimal Plc, manufacturers of vascular access devices; from the Northumbria Partnership, a patient safety collaborative; and, where annual leave or other income was compromised in fulfilling his charity duties, from the UK Sepsis Trust. RD has received sponsorship to attend and speak at one meeting from Abbott Diagnostics. He is CEO of the UK Sepsis Trust and Global Sepsis Alliance, and advises HM Government, the World Health Organization, and NHS England on sepsis. Each of these positions demands that he express opinion on strategies around the recognition and management of sepsis. MIK is a national clinical advisor on sepsis to NHS England and a national clinical advisor on deterioration to NHS Improvement. He was reimbursed for a slide set by Relias Learning. AS is the clinical fellow to the National Medical Director at NHS Improvement. AS has been sponsored on two occasions by Dr Falk Pharma UK to attend specialist gastroenterology conferences abroad; there was no contractual obligation to disseminate product information. TN is a clinical adviser to the UK Sepsis Trust. EB, LR, and PK declare that they have no competing interests.
Peer reviewers
Steven M. Opal, MD, FIDSA
Professor of Medicine
Infectious Disease Division
Rhode Island Hospital
Alpert Medical School of Brown University
Providence, RI
Disclosures
SMO declares that he has no competing interests.
Laura Evans, MD, MSc, FCCP, FCCM
Associate Professor
NYU School of Medicine
Medical Director of Critical Care
Bellevue Hospital Center
New York, NY
Disclosures
LE serves as the guidelines co-chair and on the steering committee of the Surviving Sepsis Campaign.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Singer M, Deutschman CS, Seymour CW, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA. 2016 Feb 23;315(8):801-10.Full text Abstract
Evans L, Rhodes A, Alhazzani W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Crit Care Med. 2021 Nov 1;49(11):e1063-143.Full text Abstract
National Institute for Health and Care Excellence. Suspected sepsis: recognition, diagnosis and early management. March 2024 [internet publication].Full text
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Noninfectious causes of systemic inflammatory response syndrome (SIRS)
- Myocardial infarction (MI)
- Pericarditis
More DifferentialsGuidelines
- Suspected sepsis: recognition, diagnosis and early management
- Society of Critical Care Medicine and the Infectious Diseases Society of America guidelines for evaluating new fever in adult patients in the ICU
More GuidelinesCalculators
Sequential Organ Failure Assessment: SOFA Score
APACHE II scoring system
More CalculatorsVideos
Diagnostic lumbar puncture in adults: animated demonstration
Venepuncture and phlebotomy: animated demonstration
More videosPatient information
Sepsis in adults
Pneumococcal vaccine in babies and children
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer