Summary
Definition
History and exam
Key diagnostic factors
- time taken to feed >30 minutes
- stressful mealtimes
- faltering growth (crossing downward 2 centiles)
- food refusal
- craniofacial abnormalities
- abnormal neurodevelopmental assessment
Other diagnostic factors
- inappropriate volume of feed
- vomiting
- abdominal pain, distension, or colic
- apnea, desaturations, and bradycardias in premature infants
- irritability or lethargy at mealtimes
- abnormal feeding pattern on observation
- underlying illnesses and previous hospitalizations
- previous gastrointestinal or cardiac surgery
- family history of atopy
- family history of feeding problems
- recurrent pulmonary infections and wheeze
- coughing or retching at meal times
- posture changes during feeds
- atopic features
- apparent life-threatening event (ALTEs)
- drooling
- ankyloglossia (tongue-tie)
- features of genetic conditions
Risk factors
- prematurity
- intrauterine growth restriction
- developmental delay
- anatomic abnormalities of the oropharynx or gastrointestinal tract
- gastrointestinal surgery
- neonatal cardiac surgery
- Down syndrome
Diagnostic tests
Tests to consider
- temporary exclusion of cows’ milk protein
- esophageal 24-hour pH study
- upper gastrointestinal contrast study
- esophageal impedance study
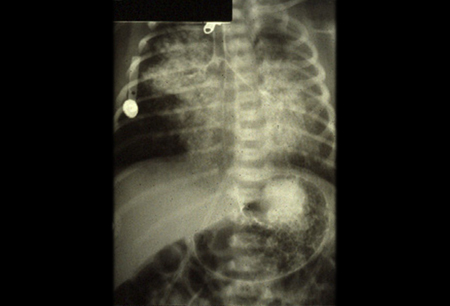
- CXR
- videofluoroscopic swallow
- fiberoptic endoscopic evaluation of swallowing with sensory testing
- upper gastrointestinal endoscopy with biopsy
- radioallergosorbent testing (RAST) to cows' milk protein
- trial of lactose-free diet
- fecal-reducing substances
- tissue transglutaminase (TTG) antibodies and total IgA
Treatment algorithm
anatomic abnormalities
gastrointestinal disorders
short bowel syndrome
neurologic impairment
prematurity
respiratory disorders
cardiac disorders
behavioral problems
Contributors
Authors
Helen McElroy, MBChB, MSc, FRCPCH
Consultant Neonatologist
Medway NHS Foundation Trust
Gillingham
Kent
UK
Disclosures
HM declares that she has no competing interests.
Acknowledgements
Dr Helen McElroy would like to gratefully acknowledge Dr Stephanie Gill and Dr Uma Sothinathan, previous contributors to this topic.
Disclosures
SG and US declare that they have no competing interests.
Peer reviewers
Alexander K.C. Leung, MBBS
Pediatric Consultant
Alberta Children's Hospital
University of Calgary
Alberta
Canada
Disclosures
AKCL declares that he has no competing interests.
Sarah N. Taylor, MD
Assistant Professor
Division of Neonatology
Medical University of South Carolina
Children's Hospital
Charleston
SC
Disclosures
SNT declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Rommel N, De Meyer AM, Feenstra L, et al. The complexity of feeding problems in 700 infants and young children presenting to a tertiary care institution. J Pediatr Gastroenterol Nutr. 2003 Jul;37(1):75-84. Abstract
Arvedson JC. Assessment of pediatric dysphagia and feeding disorders: clinical and instrumental approaches. Dev Disabil Res Rev. 2008;14(2):118-27. Abstract
Delaney AL, Arvedson JC. Development of swallowing and feeding: prenatal through first year of life. Dev Disabil Res Rev. 2008;14(2):105-17. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Physiological gastroesophageal reflux
- Malrotation with intermittent volvulus
- Intermittent intussusception
More DifferentialsGuidelines
- Identification and management of ankyloglossia and its effect on breastfeeding in infants: clinical report
- Gastro-oesophageal reflux disease in children and young people: diagnosis and management
More GuidelinesPatient information
Reflux in infants
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer