Summary
Differentials
Common
- Leukemia
- Metastatic malignancy
- Hodgkin lymphoma
- Non-Hodgkin lymphoma
- Miliary tuberculosis
- Disseminated intravascular coagulation (DIC)
- Post-transfusion
- Hemolysis, elevated liver enzymes, low platelet count (HELLP)
- Cardiopulmonary bypass
- Immune thrombocytopenia (ITP)
- Systemic lupus erythematosus (SLE)
- Rheumatoid arthritis
- Antiphospholipid syndrome
- HIV/AIDS
- Malaria
- Dengue fever
- Zika virus infection
- Cytomegalovirus (CMV)
- Infectious mononucleosis
- COVID-19
- Parvovirus B19
- Sepsis
- Heparin-induced thrombocytopenia (HIT)
- Antimalarials, antiseizure drugs, antibiotics, or chemotherapies
- Alcohol ingestion
- B12 deficiency
- Folate deficiency
- Gestational thrombocytopenia
- Cirrhosis
Uncommon
- Multiple myeloma
- Bone marrow fibrosis
- Thrombotic thrombocytopenic purpura (TTP)
- Hemolytic uremic syndrome (HUS)
- Sarcoidosis
- Cyclic thrombocytopenia
- Wiskott-Aldrich syndrome
- MYH9-related disorders, including May-Hegglin anomaly
- Bernard-Soulier syndrome
- Gaucher disease
- Hashimoto thyroiditis
- Aplastic anemia
- Vaccinations
- Paroxysmal nocturnal hemoglobinuria (PNH)
- Pseudothrombocytopenia
- Familial platelet disorder with germline RUNX1 mutation
- Thrombocytopenia due to germline ANKRD26 mutation
- Thrombocytopenia due to germline ETV6 mutation
Contributors
Authors
Hanny Al-Samkari, MD
Division of Hematology/Oncology
Peggy S. Blitz Endowed Chair in Hematology/Oncology
Massachusetts General Hospital
Associate Professor of Medicine
Harvard Medical School
Boston
MA
Disclosures
HA has received fees for consulting from Agios, Amgen, argenx, Alpine, Alnylam, Sobi, Pharmacosmos, Novartis and Sanofi; and received research funding to their institution from Amgen, Agios, Sobi, Novartis, and Vaderis.
Acknowledgements
Dr Hanny Al-Samkari would like to gratefully acknowledge Dr Julia T. Geyer and Dr Alan E. Lichtin, previous contributors to this topic. JTG declares that she has no competing interests. AEL is on an advisory board and has received research support from Amgen.
Peer reviewers
Roger M. Lyons, MD, FACP
Clinical Professor of Medicine
University of Texas Health Science Center
San Antonio
Cancer Care Network of South Texas
San Antonio
TX
Disclosures
RML declares that he has no competing interests.
Jeffrey S. Wasser, MD
Clinical Assistant Professor of Medicine
University of Connecticut School of Medicine
Farmington
CT
Disclosures
JSW has received research support from Amgen, Ligand Pharmaceuticals, and MGI Pharma for clinical studies in immune thrombocytopenic purpura.
Keith R. McCrae, MD
Professor of Medicine
Case Western Reserve University School of Medicine
Cleveland
OH
Disclosures
KRM declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Provan D, Arnold DM, Bussel JB, et al. Updated international consensus report on the investigation and management of primary immune thrombocytopenia. Blood Adv. 2019 Nov 26;3(22):3780-817.Full text Abstract
Cines DB, Levine LD. Thrombocytopenia in pregnancy. Blood. 2017 Nov 23;130(21):2271-7.Full text Abstract
American College of Obstetricians and Gynecologists. ACOG practice bulletin no. 207: thrombocytopenia in pregnancy. Obstet Gynecol. 2019 Mar;133(3):e181-93. Abstract
Cooper N, Ghanima W. Immune thrombocytopenia. N Engl J Med. 2019 Sep 5;381(10):945-55.Full text Abstract
Evans L, Rhodes A, Alhazzani W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Crit Care Med. 2021 Nov 1;49(11):e1063-143.Full text
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Patient information
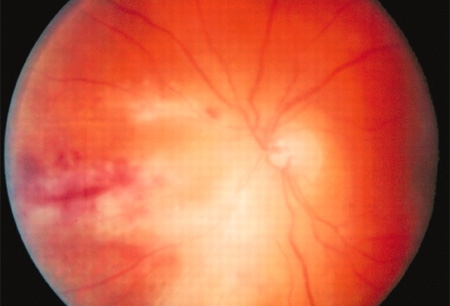
Non-Hodgkin lymphoma
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer