Summary
Definition
History and exam
Key diagnostic factors
- neonatal jaundice
- acholic stool
Other diagnostic factors
- dark urine
- bruising
- hepatomegaly
- ascites
Risk factors
- genetic predisposition
- viral infection
- environmental or behavioral exposures
Diagnostic tests
1st tests to order
- serum total and direct or conjugated bilirubin
- newborn screen (includes tests for galactosemia, thyroid dysfunction, cystic fibrosis, and a variety of metabolic diseases)
- prothrombin time (PT), INR
- CBC with differential
- serum AST, ALT, ALP, and gamma-GT
- abdominal ultrasound
Tests to consider
- hepatobiliary scintigraphy (technetium Tc 99m-di-isopropyl-acetanilido-imino-diacetic acid scan)
- liver biopsy
- cholangiogram
- CXR
- infection screen: blood and urine cultures
- urine PCR for cytomegalovirus
- plasma or serum amino acids
- alpha-1 level and protease inhibitor (Pi) type
- random serum cortisol
- urinary organic acids
- urinary succinylacetone
- urinary bile acids
- serum lactate/pyruvate ratio
Treatment algorithm
infants with biliary obstruction without end-stage liver disease
infants with biliary obstruction with end-stage liver disease
post hepatoportoenterostomy
Contributors
Authors
Kathleen Loomes, MD
Professor of Pediatrics
Department of Pediatrics
The Children's Hospital of Philadelphia
Philadelphia
PA
Disclosures
KL receives payment for contributions to UpToDate. KL has done consulting work and received research grants for clinical trials from Ipsen (formerly Albireo; manufacturer of odevixibat) and Mirum Pharmaceuticals (manufacturer of maralixibat).
Acknowledgements
Dr Kathleen Loomes would like to gratefully acknowledge Jessi Erlichman, Dr Jonathan A. Flick and Dr Barbara A. Haber, previous contributors to this topic.
Disclosures
JE declared receiving payment for contributions to UpToDate. JAF and BAH declared that they had no competing interests.
Peer reviewers
Benjamin L. Shneider, MD
Professor of Pediatrics
Service Chief in Pediatric Gastroenterology, Hepatology and Nutrition
Baylor College of Medicine
Texas Children’s Hospital
Houston
TX
Disclosures
BLS has received research funding from, and been a consultant to, several pharmaceutical companies that make antibiotic agents that might be used for treating bacterial prostatitis.
Mark D. Stringer, MD
Former Professor of Paediatric Surgery
University of Otago
Dunedin
New Zealand
Disclosures
MDS declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Harpavat S, Aucott SW, Karpen SJ, et al. Guidance for the primary care provider in identifying infants with biliary atresia by 2-4 weeks of life: clinical report. 2025 Feb 18:e2024070077.Full text Abstract
Fawaz R, Baumann U, Ekong U, et al. Guideline for the evaluation of cholestatic jaundice in infants: joint recommendations of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition. J Pediatr Gastroenterol Nutr. 2017 Jan;64(1):154-68.Full text Abstract
Squires RH, Ng V, Romero R, et al. Evaluation of the pediatric patient for liver transplantation: 2014 practice guideline by the American Association for the Study of Liver Diseases, American Society of Transplantation and the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition. Hepatology. 2014;60:362-98.Full text
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
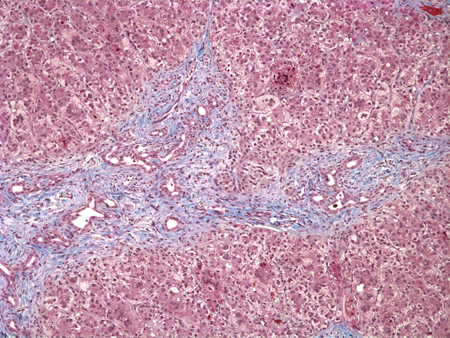
Diferenciales
- Extrahepatic biliary obstruction (e.g., choledochal cyst, spontaneous perforation of common bile duct, bile duct stricture or tumor, neonatal sclerosing cholangitis)
- Hepatic viral infections (e.g., CMV, enterovirus, HSV, echovirus, adenovirus, hepatitis B virus, HIV, rubella, reovirus type 3, parvovirus B19, EBV)
- Alagille syndrome
More DiferencialesGuías de práctica clínica
- Guidance for the primary care provider in identifying infants with biliary atresia by 2-4 weeks of life: clinical report
- Nutrition support of children with chronic liver diseases: a joint position paper of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition
More Guías de práctica clínicaFolletos para el paciente
Jaundice in newborn babies
Más Folletos para el pacienteInicie sesión o suscríbase para acceder a todo el BMJ Best Practice
El uso de este contenido está sujeto a nuestra cláusula de exención de responsabilidad