Summary
Definition
History and exam
Key diagnostic factors
- recent sinus infection
- recent eyelid injury
- redness and swelling of eye
- ocular pain
- decreased vision
- proptosis
- eyelid edema
- insect bite on eyelid
- stye or chalazion
- ear or facial infection
- ophthalmoplegia and diplopia
Other diagnostic factors
- orbital trauma
- skin infection
- chemosis
- tenderness around eye
- fever
- eyelid erythema
- elevated intraocular pressure
- headache
- malaise
- previous dental infection or dental work
- orbital fracture
- foreign body in eye or orbit
- drowsiness
- nausea/vomiting
- nasal discharge
Risk factors
- sinusitis
- young age
- male sex
- lack of Hib vaccine in children
Diagnostic tests
1st tests to order
- clinical exam
- CT sinus and orbits with contrast medium
- WBC count
Tests to consider
- blood culture
- microbiology swabs (conjunctiva, nasopharnyx, external wounds)
- MRI head and orbits with contrast medium
- Orbital ultrasonography
- lumbar puncture
Treatment algorithm
periorbital cellulitis: causative organism not identified
periorbital cellulitis: causative organism identified
orbital cellulitis: causative organism not identified
orbital cellulitis: causative organism identified
Contributors
Authors
Sudarshan Srivatsan, MD
Oculoplastics Fellow
Moran Eye Center
University of Utah
Salt Lake City
UT
Disclosures
SS declares that he has no competing interests.
Robert Kersten, MD, FACS, FASOPRS
Professor of Clinical Ophthalmology
Division Chief, Oculoplastics
Moran Eye Center
University of Utah
Salt Lake City
UT
Disclosures
RK declares that he has no competing interests.
Acknowledgements
Dr Sudarshan Srivatsan and Dr Robert Kersten would like to gratefully acknowledge Dr Sandra Lora Cremers, Dr Sarosh Janjua, and Dr H. Jane Kim, previous contributors to this topic. SLC, SJ and HJK declare that they have no competing interests.
Peer reviewers
David M. Ozog, MD
Director of Cosmetic Dermatology
Department of Dermatology
Cosmetic and Procedural Dermatology
Henry Ford Health System
Detroit
MI
Disclosures
DMO declares that he has no competing interests.
I-Hui (Elaine) Wu, MD
Resident
Wilmer Eye Institute
Baltimore
MD
Disclosures
IW declares that she has no competing interests.
Cristine Radojicic, MD
Staff Physician
Cleveland Clinic
Cleveland
OH
Disclosures
CR declares that she has no competing interests.
Jonathan Smith, MD
Specialist Registrar in Ophthalmology
Royal Victoria Infirmary
Newcastle
UK
Disclosures
JS declares that he has no competing interests.
References
Key articles
Robinson A, Beech T, McDermott AL, et al. Investigation and management of adult periorbital or orbital cellulitis. J Laryngol Otol. 2007;121:545-7. Abstract
Chandler JR, Langenbrunner DJ, Stevens ER. The pathogenesis of orbital complications in acute sinusitis. Laryngoscope. 1970;80:1414-1428. Abstract
Hamed-Azzam S, AlHashash I, Briscoe D, et al. Common orbital infections ~ state of the art ~ Part I. J Ophthalmic Vis Res. 2018 Apr-Jun;13(2):175-82.Full text Abstract
American Academy of Ophthalmology. Orbital cellulitis. Apr 2024 [internet publication].Full text
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
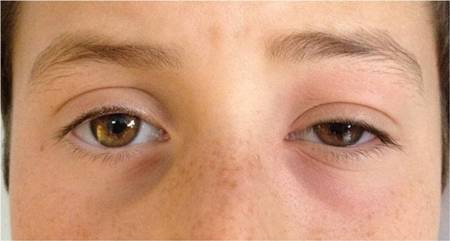
Differentials
- Orbital pseudotumor (idiopathic orbital inflammation)
- Thyroid eye disease
- Panophthalmitis
More DifferentialsGuidelines
- Guide to utilization of the microbiology laboratory for diagnosis of infectious diseases: 2024 update by the Infectious Diseases Society of America (IDSA) and the American Society for Microbiology (ASM)
- Appropriateness criteria: orbital imaging and visual loss - child
More GuidelinesPatient information
Cellulitis and erysipelas
Sinusitis
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer