Limp
Limp is defined as an asymmetric gait, and is a deviation from the normal gait pattern expected for a child's age. Causes can vary from benign to potentially life-threatening (e.g., infection, tumors, nonaccidental injury). Appropriate evaluation requires an understanding and knowledge of normal and abnormal gait patterns, potential causes, and "red flags".[1]Beresford MW, Cleary AG. Evaluation of a limping child. Curr Pediatr. 2005 Feb 1;15(1):15-22.[2]Payares-Lizano M. The limping child. Pediatr Clin North Am. 2020 Feb;67(1):119-38.
http://www.ncbi.nlm.nih.gov/pubmed/31779828?tool=bestpractice.com
The assessment of limp will depend on whether the presentation is acute or chronic.[3]Kimura Y. Common presenting problems. In: Arthritis in children and adolescents: juvenile idiopathic arthritis. Szer I, Kimura Y, Malleson PN, et al (eds). Oxford: Oxford University Press; 2006:24-48.
Trauma, causing transient injury, is the most common cause of limp, although the potential for serious or life-threatening causes requires a thorough clinical assessment and appropriate investigations.[2]Payares-Lizano M. The limping child. Pediatr Clin North Am. 2020 Feb;67(1):119-38.
http://www.ncbi.nlm.nih.gov/pubmed/31779828?tool=bestpractice.com
Challenges in making a diagnosis include the complexity of history taking in the pediatric setting. Often, the history is taken from the caregiver, and the trauma may have occurred in a childcare setting, rather than at home. The history may therefore be vague and inaccurate.
Careful examination of all joints is necessary, as is general assessment including abdominal, neurologic, and developmental assessments.[4]Foster HE, Cabral DA. Is musculoskeletal history and examination so different in paediatrics? Best Pract Res Clin Rheumatol. 2006 Apr;20(2):241-62.
https://www.sciencedirect.com/science/article/abs/pii/S1521694205001245?via%3Dihub
http://www.ncbi.nlm.nih.gov/pubmed/16546055?tool=bestpractice.com
Normal motor milestones
[Figure caption and citation for the preceding image starts]: Normal motor milestones [Citation ends].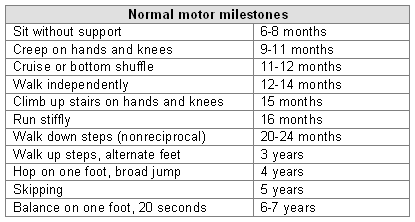
Persisting primitive reflexes beyond 6 months are suggestive of neurologic problems such as cerebral palsy.
Normal gait patterns
The toddler has a broad base gait for support, and appears to be high stepped and flat footed, with arms outstretched for balance. The legs are externally rotated, with a degree of bowing. Heel strike develops at around 15 to 18 months with reciprocal arm swing. Running and change of direction occur after the age of 2 years.
In the school-age child, the step length increases and step frequency slows. Adult gait and posture occur around the age of 8 years. There is considerable variation in normal gait patterns, and the ages at which the changes occur, that appear to be family-history related.
Normal variations
Leg alignment varies with age and is often influenced by a family history of the same pattern.[5]Sass P, Hassan G. Lower extremity abnormalities in children. Am Fam Physician. 2003 Aug 1;68(3):461-8.
https://www.aafp.org/afp/2003/0801/p461.html
http://www.ncbi.nlm.nih.gov/pubmed/12924829?tool=bestpractice.com
Habitual toe walking is common in young children up to 3 years. In-toeing can be due to persistent femoral anteversion and is characterized by the child walking with patellae and feet pointing inward (common between the ages of 3 and 8 years).
Internal tibial torsion is characterized by the child walking with patella facing forward and toes pointing inward (common from onset of walking to 3 years).
Metatarsus adductus is characterized by a flexible "C-shaped" lateral border of the foot. Most resolve by the age of 6 years.
Bow legs (genu varum) are common from birth to early toddlerhood, often with out-toeing (maximal at approximately 1 year). Most resolve by 18 months.
Knock knees (genu valgum). Often associated with in-toeing. Most resolve by the age of 7 years.
Flat feet. Most children have a flexible foot with normal arch on tiptoeing. Flat feet usually resolve by the age of 6 years.[Figure caption and citation for the preceding image starts]: Flat feet and normal arches on tip toeFrom Dr Foster's personal collection; used with permission [Citation ends].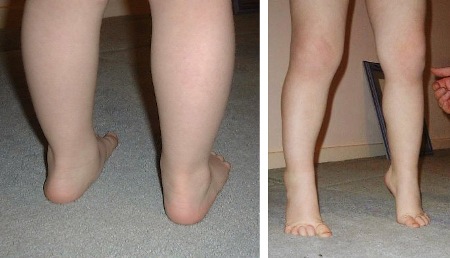
Crooked toes. Most resolve with weight-bearing.
Causes for concern arise if these normal variations are persistent (i.e., beyond the expected age range), if changes are progressive or asymmetric, or if there is pain and functional limitation or evidence of neurologic disease.
In children with bow legs or knock knees, it is important to consider x-rays if the child is short (a height less than the 25th centile raises suspicions of hypophosphatemic rickets or skeletal dysplasias) or has genu varum or asymmetric leg alignment.[6]Greene WB. Genu varum and genu valgum in children: differential diagnosis and guidelines for evaluation. Compr Ther. 1996 Jan;22(1):22-9.
http://www.ncbi.nlm.nih.gov/pubmed/8654021?tool=bestpractice.com
Abnormal gait patterns
Antalgic gait
Reduced time spent weight-bearing on the affected side.
Spectrum of possible causes (e.g., trauma to sole of foot, spinal osteomyelitis). Unwitnessed trauma is common in young children. The child presents with unwillingness to weight-bear, so an index of suspicion is required.
May be observed in juvenile idiopathic arthritis (JIA), although children may not always complain of pain.[7]McGhee JL, Burks FN, Sheckels JL, et al. Identifying children with chronic arthritis based on chief complaints: absence of predictive value for musculoskeletal pain as an indicator of rheumatic disease in children. Pediatrics. 2002 Aug;110(2 Pt 1):354-9.9.
https://pediatrics.aappublications.org/content/110/2/354.long
http://www.ncbi.nlm.nih.gov/pubmed/12165590?tool=bestpractice.com
Circumduction gait ("peg leg")
Excessive hip abduction as the leg swings forward.
Typically seen with a leg length discrepancy, with a stiff/restricted joint movement as in JIA, or with unilateral spasticity as in hemiplegic cerebral palsy.
Spastic gait
Stiff, foot-dragging with foot inversion. This is often seen in upper motor neuron neurologic disease (e.g., diplegic or quadriplegic cerebral palsy, stroke).
Ataxic gait
Instability with an alternating narrow to wide base of gait.
Seen in conditions affecting the cerebellum (e.g., acute cerebellitis, posterior fossa tumor, ataxic cerebral palsy).
May also be due to a sensory ataxia, found in conditions affecting proprioception, such as sensory neuropathies.
Trendelenberg gait
Results from hip abductor muscle weakness. While weight-bearing on the ipsilateral side, the pelvis drops on the contralateral side, rather than rising as is normal. With bilateral hip disease, this results in a waddling "rolling sailor" gait with hips, knees, and feet externally rotated.
May be observed in Legge-Calve-Perthes disease, slipped capital femoral epiphysis, developmental dysplasia of the hip, JIA involving the hip, muscle disease (juvenile dermatomyositis or inherited myopathies), and neurologic conditions (spina bifida, cerebral palsy, and spinal cord injury).
Toe-walking gait ("equinus") with absent heel contact
Habitual toe walking is common in normal children and associates with normal tone, range of movement around the feet, and normal walking on request. However, persistent toe walking is observed in spastic upper motor neuron neurologic disease (e.g., diplegic cerebral palsy) and may be a presentation of mild lysosomal storage disorder.
Stepping gait
The entire leg is lifted at the hip to assist with ground clearance. Occurs with weak ankle dorsiflexors, compensated by increased knee flexion (i.e., a foot drop gait).
Observed in lower motor neuron neurologic disease and conditions affecting the nerve root (e.g., spina bifida) and peripheral neuropathies (e.g., Charcot-Marie-Tooth disease, Guillain-Barre syndrome).
"Clumsy" gait
This term is commonly used to describe difficulties in motor coordination (fine and gross motor skills). The child may present with frequent falls, difficulty in self-help skills such as dressing or feeding at school. Poor handwriting and learning disabilities may be noted.
It is important to exclude specific albeit mild neurologic disabilities (cerebral palsy, cerebellar ataxia, or lower motor neuron disorders), indolent inflammatory arthritis or myopathies, and orthopedic problems such as in-toeing. Metabolic disorders that may present with "clumsy walking" should also be considered.


