Summary
Definition
History and exam
Key diagnostic factors
- risk factors for sexually transmitted infection (STI)
- purulent vaginal or cervical discharge
- intermenstrual/postcoital bleeding
- dysuria and urinary frequency
- easily induced cervical bleeding
Other diagnostic factors
- dyspareunia
- vulval and/or vaginal inflammation
- strawberry cervix
Risk factors
- age 15 to 24 years
- inconsistent condom use
- multiple sexual relationships
- previous STIs
- bacterial vaginosis (BV)
- sex worker
- absence of hydrogen peroxide-producing lactobacilli
- infertility
- education <12 years
Diagnostic tests
1st tests to order
- pregnancy test
- wet mount examination of cervical discharge
- nucleic acid amplification testing (NAAT)
- rapid tests (OSOM Trichomonas, AFFIRM VPIII)
- Thayer-Martin agar cervical culture
- Gram stain of cervical discharge
Tests to consider
- cervical cytology
- herpes simplex virus (HSV) serology
- HIV serology
- hepatitis B and C serologies
- rapid plasma reagin testing
Treatment algorithm
high-risk nonpregnant women
nonpregnant women
pregnant women
recurrent/resistant infections
Contributors
Authors
M. Jonathon Solnik, MD, FACOG, FACS

Associate Professor of Obstetrics & Gynaecology
Head of Gynaecology & Minimally Invasive Surgery
University of Toronto Faculty of Medicine
Mount Sinai Hospital
Toronto
Canada
Disclosures
MJS serves as a consultant for Medtronic, Olympus, and Hologic, and on the advisory board for Abbvie. He holds stocks in Felix and Field Trip Inc.
Acknowledgements
Dr M. Jonathon Solnik would like to gratefully acknowledge Dr Sharon Jakus, a previous contributor to this topic.
Disclosures
SJ declares that she has no competing interests.
Peer reviewers
Sandra R. Valaitis, MD
Associate Professor and Chief
Gynecology and Reconstructive Pelvic Surgery
University of Chicago
Chicago
IL
Disclosures
SRV declares that she has no competing interests.
Justin C. Chura, MD
Associate Division Director
Gynecologic Oncology
Crozer Chester Medical Center
Upland
PA
Disclosures
JCC declares that he has no competing interests.
Eva Jungmann, FRCP, MSc
Consultant Physician
GUM/HIV Camden Primary Care Trust
Archway Sexual Health Clinic
London
UK
Disclosures
EJ declares that she has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021 Jul 23;70(4):1-187.Full text Abstract
Boyer CB, Shafer MB, Pollack LM, et al. Sociodemographic markers and behavioral correlates of STIs in a nonclinical sample of adolescent and young adult women. J Infect Dis. 2006 Aug 1;194(3):307-15.Full text Abstract
Marrazzo JM, Weisenfeld HC, Murray PJ, et al. Risk factors for cervicitis among women with bacterial vaginosis. J Infect Dis. 2006 Mar 1;193(5):617-24.Full text Abstract
Scholes D, Grothaus L, McClure J, et al. A randomized trial of strategies to increase Chlamydia screening in young women. Prev Med. 2006 Oct;43(4):343-50. Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
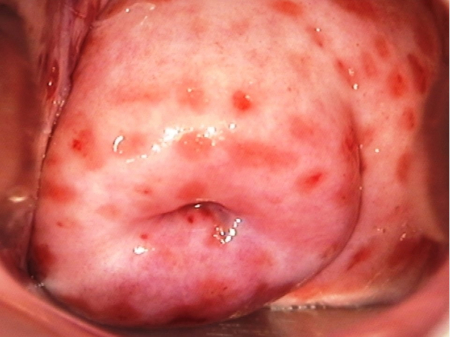
Differentials
- Cervical ectropion
- Cervical dysplasia
- Cervical cancer
More DifferentialsGuidelines
- European guideline on the management of Mycoplasma genitalium infections
- British Association for Sexual Health and HIV (BASHH) United Kingdom national guideline on the management of Trichomonas vaginalis 2021
More GuidelinesPatient information
Chlamydia
Genital herpes
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer