An important nail sign of systemic disease linked with underlying pulmonary, cardiovascular, neoplastic, infectious, hepatobiliary, mediastinal, endocrine, and gastrointestinal disorders.
Definition
Clubbing is a bulbous uniform swelling of the soft tissue of the terminal phalanx of a digit with subsequent loss of the normal angle between the nail and nail bed.
The first stage of clubbing is a periungual erythema and a softening of the nail bed; this is followed by an increase in the Lovibond angle (the angle between the proximal nail fold and the nail plate). Eventually the depth of the distal phalanx increases and the distal interphalangeal joint may become hyperextensible.[1]Marrie TJ, Brown N. Clubbing of the digits. Am J Med. 2007 Nov;120(11):940-1.
http://www.ncbi.nlm.nih.gov/pubmed/17976417?tool=bestpractice.com
[2]Sarkar M, Mahesh DM, Madabhavi I. Digital clubbing. Lung India. 2012 Oct;29(4):354-62.
https://www.doi.org/10.4103/0970-2113.102824
http://www.ncbi.nlm.nih.gov/pubmed/23243350?tool=bestpractice.com
The Schamroth window test can be used to identify or confirm clubbing. If 2 opposing fingers are held back to back against each other, a diamond-shaped space should normally appear between the nail beds and the nails of the 2 fingers. In clubbing, this space (or window) is missing. [Figure caption and citation for the preceding image starts]: Schamroth window test demonstrating a diamond-shaped window when fingers are not clubbedCreated by BMJ Knowledge Centre [Citation ends].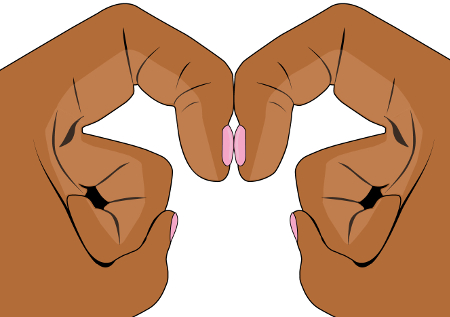 [Figure caption and citation for the preceding image starts]: Schamroth window test demonstrating lack of window with clubbed fingersCreated by BMJ Knowledge Centre [Citation ends].
[Figure caption and citation for the preceding image starts]: Schamroth window test demonstrating lack of window with clubbed fingersCreated by BMJ Knowledge Centre [Citation ends].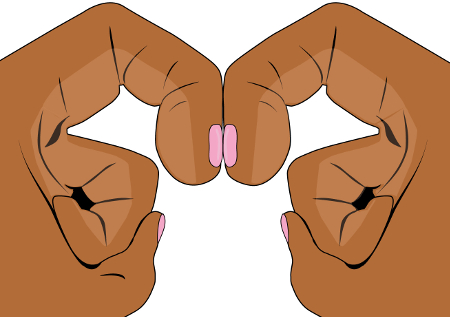
Clubbing is usually bilateral, although unilateral clubbing does exist (e.g., axillary artery aneurysm and brachial arteriovenous malformations). It is painless unless associated with underlying conditions such as pulmonary hypertrophic osteoarthropathy. The vast majority of patients are unaware of its presence. However, an understanding of the causation and diseases associated with clubbing alerts the physician to the seriousness of this sign and the need to investigate the patient appropriately.[Figure caption and citation for the preceding image starts]: Finger clubbingFrom the collection of Dr Murlidhar Rajagopalan [Citation ends]. [Figure caption and citation for the preceding image starts]: Pachydermoperiostosis: toe clubbingFrom the collection of Dr Murlidhar Rajagopalan [Citation ends].
[Figure caption and citation for the preceding image starts]: Pachydermoperiostosis: toe clubbingFrom the collection of Dr Murlidhar Rajagopalan [Citation ends].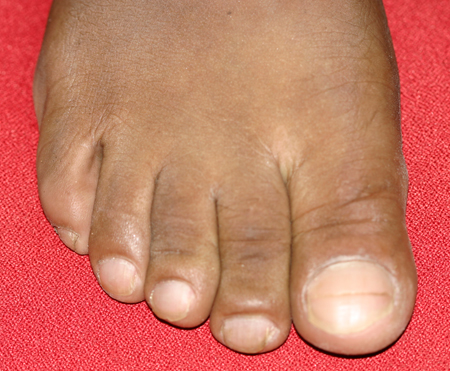 [Figure caption and citation for the preceding image starts]: Clubbing of nails showing loss of the classic Lovibond angle (normally ≤160° in a normal distal digit, but >180° with definitive clubbing)From the collection of Dr Murlidhar Rajagopalan [Citation ends].
[Figure caption and citation for the preceding image starts]: Clubbing of nails showing loss of the classic Lovibond angle (normally ≤160° in a normal distal digit, but >180° with definitive clubbing)From the collection of Dr Murlidhar Rajagopalan [Citation ends].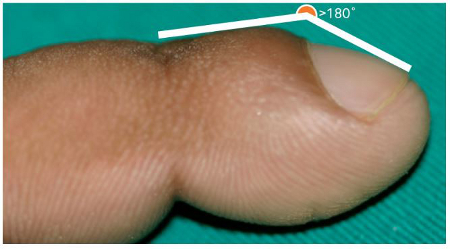
Pathophysiology
Vascular endothelial growth factor (VEGF) is key.[3]Callemeyn J, Van Haecke P, Peetermans WE, et al. Clubbing and hypertrophic osteoarthropathy: insights in diagnosis, pathophysiology, and clinical significance. Acta Clin Belg. 2016 Jun;71(3):123-30.
http://www.ncbi.nlm.nih.gov/pubmed/27104368?tool=bestpractice.com
This platelet-derived factor is stimulated by hypoxia and produced in diverse malignancies and conditions that affect circulation. VEGF induces vascular hyperplasia, edema, and fibroblast or osteoblast proliferation at a peripheral level in the nails. In primary pulmonary conditions such as lung cancer, this is the operative mechanism. When there is extrapulmonary shunting of blood - for example, in cyanotic heart disease - large megakaryocytic fragments gain access to the systemic circulation and affect distal sites such as the nails. Here, these fragments release growth factors, including VEGF.[1]Marrie TJ, Brown N. Clubbing of the digits. Am J Med. 2007 Nov;120(11):940-1.
http://www.ncbi.nlm.nih.gov/pubmed/17976417?tool=bestpractice.com
[4]Martinez-Lavin M. Exploring the cause of the most ancient clinical sign of medicine: finger clubbing. Semin Arthritis Rheum. 2007 Jun;36(6):380-5.
http://www.ncbi.nlm.nih.gov/pubmed/17276498?tool=bestpractice.com
In cases of bronchogenic carcinoma, growth hormone has been implicated as a cause of clubbing. In hypertrophic osteoarthropathy, an additional unknown factor is considered necessary to produce this syndrome; cyanosis may also be required.[5]Dickinson CJ, Martin JF. Megakaryocytes and platelet clumps as the cause of finger clubbing. Lancet. 1987 Dec 19;2(8573):1434-5.
http://www.ncbi.nlm.nih.gov/pubmed/2891996?tool=bestpractice.com
[6]Silveira LH, Martinez-Levin M, Pineda C, et al. Vascular endothelial growth factor and hypertrophic osteoarthropathy. Clin Exp Rheumatol. 2000 Jan-Feb;18(1):57-62.
http://www.ncbi.nlm.nih.gov/pubmed/10728444?tool=bestpractice.com
Hypertrophic osteoarthropathy is characterized by abnormal proliferation of skin and periosteal tissues involving the extremities and is clinically evident as digital clubbing, periostosis of tubular bones, and synovial effusions.[7]Yap FY, Skalski MR, Patel DB, et al. Hypertrophic osteoarthropathy: clinical and imaging features. Radiographics. 2017 Jan-Feb;37(1):157-95.
http://www.ncbi.nlm.nih.gov/pubmed/27935768?tool=bestpractice.com
Platelet derived growth factor (PDGF) likely plays a role in the pathogenesis of clubbing.[2]Sarkar M, Mahesh DM, Madabhavi I. Digital clubbing. Lung India. 2012 Oct;29(4):354-62.
https://www.doi.org/10.4103/0970-2113.102824
http://www.ncbi.nlm.nih.gov/pubmed/23243350?tool=bestpractice.com
[8]Atkinson S, Fox SB. Vascular endothelial growth factor (VEGF)-A and platelet-derived growth factor (PDGF) play a central role in the pathogenesis of digital clubbing. J Pathol. 2004 Jun;203(2):721-8.
http://www.ncbi.nlm.nih.gov/pubmed/15141388?tool=bestpractice.com
Platelets release PDGF in the vasculature of the fingertips. Conditions that involve chronic platelet excess (e.g., inflammatory bowel disease) result in peripheral platelet trapping and release of PDGF.[5]Dickinson CJ, Martin JF. Megakaryocytes and platelet clumps as the cause of finger clubbing. Lancet. 1987 Dec 19;2(8573):1434-5.
http://www.ncbi.nlm.nih.gov/pubmed/2891996?tool=bestpractice.com
PDGF stimulates growth, vascular permeability, and monocyte and neutrophil chemotaxis, and leads to proliferation of vascular smooth muscle cells and fibroblasts, as is seen in clubbing.[5]Dickinson CJ, Martin JF. Megakaryocytes and platelet clumps as the cause of finger clubbing. Lancet. 1987 Dec 19;2(8573):1434-5.
http://www.ncbi.nlm.nih.gov/pubmed/2891996?tool=bestpractice.com
Clubbing may be stimulated by local arteriovenous anastomoses provoked by neurocirculatory stimuli. Unilateral clubbing secondary to local disorders (e.g., axillary artery aneurysm) is not due to a pulmonary circulation defect.[9]Kahtan S, Kahtan N. Unilateral finger clubbing. Lancet. 1991 Aug 31;338(8766):576.
http://www.ncbi.nlm.nih.gov/pubmed/1678833?tool=bestpractice.com
[10]Kinjo T, Arakaki W, Fujita J. Unilateral digital clubbing in hemiplegia due to a putaminal hemorrhage. Clin Case Rep. 2022 Mar 1;10(3):e05519.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8888808
http://www.ncbi.nlm.nih.gov/pubmed/35261774?tool=bestpractice.com



Log in or subscribe to access all of BMJ Best Practice



