Summary
Definition
History and exam
Other diagnostic factors
- dyspnea
- decreased exercise tolerance
- diastolic murmur
- orthopnea
- paroxysmal nocturnal dyspnea
- palpitations
- fatigue
- diaphoresis
- displaced point of maximal apical impulse
- systolic murmur
- signs of right-sided heart failure
Risk factors
- pulmonary hypertension
- surgical repair of tetralogy of Fallot, pulmonary stenosis, or pulmonary atresia
- endocarditis
- left-sided heart disease
- previous Ross procedure (with prosthetic pulmonary valve, homograft valve replacement)
- collagen vascular disease
- malignancies that involve the main pulmonary artery
Diagnostic tests
1st tests to order
- ECG
- transthoracic Doppler echocardiogram (TTE)
- CXR
Tests to consider
- transesophageal Doppler echocardiogram (TEE)
- cardiac MRI
- MRI chest
- CT scan chest
Treatment algorithm
acute pulmonary regurgitation
chronic pulmonary regurgitation
Contributors
Authors
Karen K. Stout, MD, FACC
Professor of Medicine
Adjunct Professor of Pediatrics and Cardiology
Division of Cardiology
University of Washington
Seattle
WA
Disclosures
KKS is former chair of a prior ACC/AHA guidelines committee and an author of a guideline cited in this topic.
Andrew Pistner, MD
Assistant Professor of Medicine
Division of Cardiology
University of Washington
Seattle
WA
Disclosures
AP declares that he has no competing interests.
Acknowledgements
Dr Karen K. Stout and Dr Andrew Pistner would like to gratefully acknowledge Dr Sachin S. Goel, Dr Chetan P. Huded, Dr Samir Kapadia, and Dr Mehdi H. Shishehbor, previous contributors to this topic.
Disclosures
SSG, CPH, SK, and MHS declare that they have no competing interests.
Peer reviewers
Satish Adwani, MD
Consultant in Paediatric Cardiology and Adults with Congenital Heart Disease
John Radcliffe Hospital
Oxford
UK
Disclosures
SA declares that he has no competing interests.
Sarabjeet Singh, MD
Cardiology Fellow
Adult Cardiovascular Fellowship
Department of Cardiology
Chicago Medical School (CMS) and affiliated hospitals
Chicago
IL
Disclosures
SS declares that he has no competing interests.
Debabrata Mukherjee, MD
Gill Foundation Professor of Interventional Cardiology
Director of Cardiac Catheterization Laboratories
Gill Heart Institute
Division of Cardiovascular Medicine
University of Kentucky
Lexington
KY
Disclosures
DM declares that he has no competing interests.
Syed Wamique Yusuf, MD, MRCPI, FACC
Associate Professor
University of Texas MD Anderson Cancer Center
Department of Cardiology
Houston
TX
Disclosures
SWY declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
American College of Radiology. ACR appropriateness criteria: congenital or acquired heart disease. 2023 [internet publication].Full text
Writing Committee Members, Otto CM, Nishimura RA, et al. 2020 ACC/AHA guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2021 Feb 2;77(4):e25-197.Full text Abstract
Stout KK, Daniels CJ, Aboulhosn JA, et al. 2018 AHA/ACC guideline for the management of adults with congenital heart disease: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. J Am Coll Cardiol. 2019 Apr 2;73(12):e81-192.Full text Abstract
Baumgartner H, De Backer J, Babu-Narayan SV, et al. 2020 ESC guidelines for the management of adult congenital heart disease. Eur Heart J. 2021 Feb 11;42(6):563-645.Full text Abstract
Bokma JP, Geva T, Sleeper LA, et al. Improved outcomes after pulmonary valve replacement in repaired tetralogy of Fallot. J Am Coll Cardiol. 2023 May 30;81(21):2075-85.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Mitral stenosis
- Aortic regurgitation (AR)
- Atrial myxoma
More DifferentialsGuidelines
- ACR appropriateness criteria: known or suspected congenital heart disease
- ACR appropriateness criteria: known or suspected congenital heart disease
More GuidelinesPatient information
Heart failure
Heart failure: how can I help myself?
More Patient informationVideos
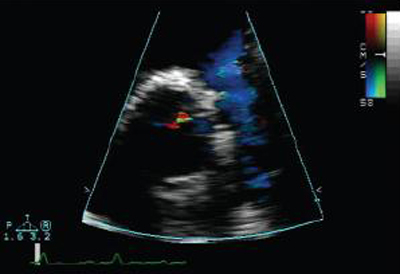
Pulmonary regurgitation
More videosLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer