Epidemiology
Meningitis causes hundreds of thousands of deaths globally each year. Although viral meningitis is more common than bacterial meningitis, bacterial meningitis is more likely to be associated with a poor prognosis, higher mortality, and requires prompt recognition and treatment.[5][6]
The Global Burden of Disease Study estimated that in 2019 there were 236,000 deaths globally due to meningitis.[5] The most common bacterial meningitis etiologies in all regions globally were Streptococcus pneumoniae, Neisseria meningitidis (or meningococcus), Haemophilus influenzae, and Streptococcus agalactiae (group B streptococcus). These bacteria are responsible for more than half the deaths from meningitis globally. S pneumoniae was the leading cause of all age meningitis deaths at 18.1%. Although vaccines can prevent most infections due to these three etiologies, not all countries have fully immunized their populations.[5][7]
The epidemiology of bacterial meningitis has changed due to widespread immunization programs, including the introduction of protein-polysaccharide conjugate vaccines. In countries with universal Haemophilus influenzae type b (Hib) immunization programs, the incidence of Hib meningitis has declined by 95% to 99%.[8][9]
Pneumococcal meningitis
S pneumoniae continues to be the leading cause of invasive bacterial meningitis globally. In the US, it accounts for approximately 2000 cases per year.[10] However, since the 2000 introduction of the heptavalent pneumococcal vaccine in the US, the overall rates of pneumococcal meningitis have declined significantly from 0.8 in 100,000 in 1997 to 0.3 in 100,000 in 2010. A further decline in pneumococcal meningitis, particularly in patients age 2 years or less, was recorded subsequent to the introduction of the 10- and 13-valent vaccines in 2010.[11][12][13]
Meningococcal meningitis
N meningitidis, causing meningococcal meningitis, is the pathogen with the most potential to produce large epidemics. There are 12 serogroups of N meningitidis that have been identified, 6 of which (A, B, C, W, X, and Y) can lead to mass outbreaks of the disease.[7] The highest incidence of meningococcal disease is found in the “meningitis belt” of sub-Saharan Africa, where rates can reach 1000 cases per 100,000 population.[14] The incidence in African countries is 10-40 in 100,000 people per year. The higher rates of infection reflect the epidemics of meningococcal meningitis that occur throughout the African meningitis belt during the dry season.[8][15][16] Globally, of the top 10 countries with the greatest absolute number of meningitis deaths, only four are located outside the African meningitis belt (India, Pakistan, Afghanistan, China).[17]
Most outbreaks of N meningitidis outside Africa are caused by meningococcal serogroups B and C, with emergence of serogroup W135 since 2012.[16] In Africa, serogroups A, C, and W account for substantial proportions of meningococcal disease.[18] Meningococcal vaccines are available for serogroups A, B, C, W, and Y.
In the US, the overall rate of meningococcal disease has been declining since the 1990s, with further declines linked to the introduction of the quadrivalent meningococcal conjugate vaccine in 2005.[19] A decrease in incidence was also witnessed in other countries with conjugated vaccine uptake. In the UK, serogroup C vaccination was implemented in 1998 and serogroup B vaccination in 2015.[20] Much of the beneficial effect of these vaccines was achieved by herd immunity.[21] However, in Europe and the UK, the incidence of invasive meningococcal disease did slightly increase from 0.1 cases per 100,000 population in 2021 to an estimated 0.3 cases per 100,000 population in 2022. There were 1149 confirmed cases of bacterial meningitis reported in the 30 European Union/European Economic Area Member States, with serotype B being the major cause (62%), followed by serotype Y (16%).[22]
In the US, the incidence of meningococcal meningitis decreased from 0.72 in 100,000 in 1997 to an historic low of 0.1 cases per 100,000 in 2018.[11][23] However, there has been a recent sharp increase in US cases since 2021, specifically attributed to a strain of serogroup Y, ST-1466. The incidence of meningococcal disease now exceeds pre-pandemic levels. In 2023, 438 confirmed and probable cases were reported. This is the largest number of US meningococcal disease annual cases reported since 2014, with N meningitidis serogroup Y responsible for much of this recent increase.[24] Per the Centers for Disease Control and Prevention, this strain was responsible for at least 68% of all serogroup Y cases reported in 2023. Cases of invasive meningococcal disease caused by this strain occurred in both males (65%) and females (35%) and disproportionately occurred in people ages 30-60 years (65%), Black or African American people (63%), and people with HIV (15%). In addition, most cases of invasive meningococcal disease caused by ST-1466 had varied clinical presentations; 64% presented with bacteremia, and at least 4% presented with septic arthritis. Of 94 patients with known outcomes, 17 (18%) died; this case-fatality rate is higher than the historic case-fatality rate of 11% reported for serogroup Y cases in 2017-2021.[25]
[Figure caption and citation for the preceding image starts]: Laboratory-confirmed cases of invasive meningococcal disease in England by capsular group and epidemiologic year. The light blue and dark blue arrows denote the start of the national immunization program against group C meningococcal (MenC) disease and group B meningococcal (MenB) disease, respectivelyPublic Health England [Citation ends].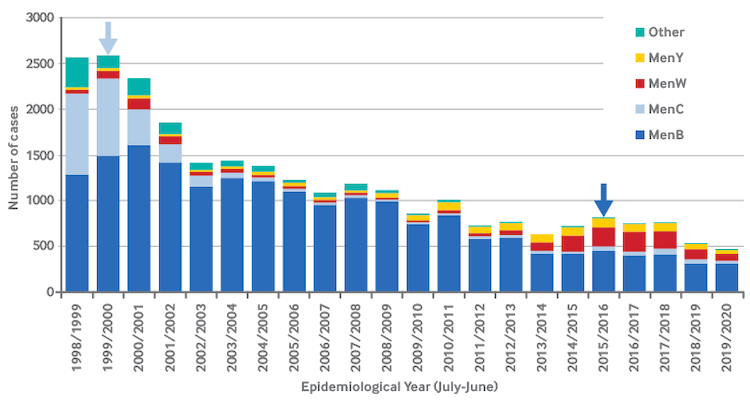
Risk factors
Risk of acquiring bacterial meningitis is increased after exposure to infection within the household or close contact with a patient who has meningitis.[1]
High risk of contracting Haemophilus influenzae type b, pneumococcal, or meningococcal meningitis.[9]
About 50% of patients with bacterial meningitis have predisposing conditions, one third of whom have an immunodeficiency.[42]
Patients with HIV infection become increasingly susceptible to bacterial meningitis, particularly if they develop AIDS. Risk is increased approximately eightfold compared with the general population.[43] Bacterial meningitis in this population is primarily caused by Streptococcus pneumoniae, but Salmonella meningitis is also possible.[43][44][45]
Congenital immunodeficiencies, such as complement deficiencies, X-linked agammaglobulinemia, immunoglobulin G subclass deficiency, or interleukin 1 receptor-associated kinase 4 deficiency, have been associated with bacterial meningitis.[46]
Increases risk of overwhelming bacterial infections with encapsulated bacteria, particularly Streptococcus pneumoniae, Neisseria meningitidis, and Haemophilus influenzae.[46]
Cochlear implant recipients are at higher risk of bacterial meningitis than the general population.[48]
Use of this content is subject to our disclaimer
