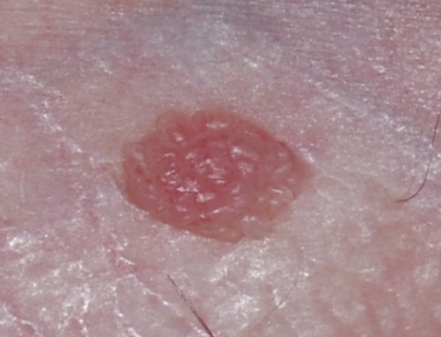
Summary
Definition
History and exam
Key diagnostic factors
- increased risk of exposure to HPV
- immunocompromise
- sessile exophytic papillomas
Other diagnostic factors
- asymptomatic
- pruritus
- bleeding
- pain
- urinary symptoms
Risk factors
- intercourse at an early age
- increasing number of lifetime sexual partners
- young sexually active adults
- increasing number of partner's lifetime sexual partners
- immunocompromise
Diagnostic tests
1st tests to order
- no initial test
Tests to avoid
- low-risk HPV testing
Tests to consider
- biopsy
- anoscopy
- urethroscopy
Treatment algorithm
nonpregnant and immunocompetent
immunocompromised
pregnant
Contributors
Authors
Natalia Mendoza, MD
Pariser Dermatology Specialist
Williamsburg
VA
Disclosures
NM declares that she has no competing interests.
Stephen K. Tyring, MD, PhD, MBA
Clinical Professor
Departments of Dermatology, Microbiology and Molecular Genetics and Internal Medicine
University of Texas Health Science Center
Houston
TX
Disclosures
SKT declares that he has no competing interests.
Acknowledgements
Dr Natalia Mendoza and Dr Stephen K. Tyring would like to gratefully acknowledge Dr Brenda L. Pellicane, a previous contributor to this topic.
Disclosures
BLP declares that she has no competing interests.
Peer reviewers
Angela Moore, MD
Clinical Assistant Professor
University of Texas Medical Branch at Galveston
Galveston
TX
Disclosures
AM declares that she has no competing interests.
Steve Baguley, FRCP, MSc
Consultant Genitourinary Physician
Woolmanhill Hospital
Aberdeen
Scotland
UK
Disclosures
SB declares that he has no competing interests.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Forcier M, Musacchio N. An overview of human papillomavirus infection for the dermatologist: disease, diagnosis, management, and prevention. Dermatol Ther. 2010 Sep-Oct;23(5):458-76. Abstract
Ahmed AM, Madkan V, Tyring SK. Human papillomaviruses and genital disease. Dermatol Clin. 2006 Apr;24(2):157-65. Abstract
Meites E, Szilagyi PG, Chesson HW, et al. Human papillomavirus vaccination for adults: updated recommendations of the Advisory Committee on Immunization Practices. MMWR Morb Mortal Wkly Rep. 2019 Aug 16;68(32):698-702.Full text Abstract
Beutner KR, Wiley DJ, Douglas JM, et al. Genital warts and their treatment. Clin Infect Dis. 1999 Jan;28 Suppl 1:S37-56. Abstract
Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021 Jul 23;70(4):1-187.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
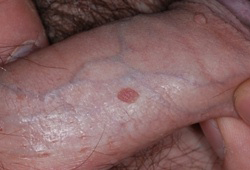
Differentials
- Condyloma latum
- Molluscum contagiosum
- Pearly penile papules
More DifferentialsGuidelines
- Guidelines for the prevention and treatment of opportunistic infections in adults and adolescents with HIV: human papillomavirus disease
- Reducing sexually transmitted infections
More GuidelinesPatient information
Genital warts
HPV (human papillomavirus) vaccine
More Patient informationLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer