Summary
Definition
History and exam
Key diagnostic factors
- fever
- decreased milk outflow
- breast warmth
- breast tenderness
- breast firmness
- breast swelling
- breast erythema
- flu-like symptoms, malaise, and myalgia
- breast pain
- breast mass
- fistula
Other diagnostic factors
- nipple discharge
- nipple inversion/retraction
- lymphadenopathy
- extra-mammary skin lesions
Risk factors
- female sex
- poor breast-feeding technique
- lactation
- milk stasis
- nipple injury
- previous mastitis
- prolonged mastitis (breast abscess)
- women aged >30 years (breast abscess)
- prior breast abscess (breast abscess)
- shaving or plucking areola hair
- anatomical breast defect, mammoplasty, or scar
- other underlying breast condition
- nipple piercing
- foreign body
- skin infection
- Staphylococcus aureus carrier
- immunosuppression
- hospital admission
- breast trauma
- primiparity (breast abscess)
- multiparity
- overabundant milk supply
- complications of delivery
- maternal stress
- tight clothing
- antifungal nipple cream
- fibrocystic breast disease
- cigarette smoking
- vaginal manipulation (breast abscess)
- antiretroviral therapy
Diagnostic tests
1st tests to order
- breast ultrasound
- diagnostic needle aspiration drainage
- cytology of nipple discharge or sample from fine-needle aspiration
- milk, aspirate, discharge, or biopsy tissue for culture and sensitivity
Tests to consider
- pregnancy test
- blood culture and sensitivity
- histopathologic examination of biopsy tissue
- mammogram
- milk for leukocyte counts and bacteria quantification
- CBC
Treatment algorithm
lactational mastitis
nonlactational mastitis
breast abscess
breast abscess post acute intervention
recurrence of mastitis and/or breast abscess
Contributors
ავტორები
Jesse Casaubon, DO, FSSO, FACS
Breast Surgical Oncologist
Baystate Health
Springfield
MA
გაფრთხილება:
JC declares that he has no competing interests.
მადლიერება
Dr Jesse Casaubon would like to gratefully acknowledge Dr Holly S. Mason, Dr Jose A. Martagon-Villamil, Dr Daniel Skiest, Dr Gina Berthold, and Dr Liron Pantanowitz, previous contributors to this topic.
გაფრთხილება:
HSM, JAMV, DS, and GB declare that they have no competing interests. LP is a co-author of references cited in this topic.
რეცენზენტები
Edward Sauter, MD, PhD
Program Officer
National Institutes of Health
National Cancer Institute
Rockville
MD
გაფრთხილება:
ES declares that he has no competing interests.
Justin Stebbing, MA, MRCP, MRCPath, PhD
Consultant Medical Oncologist/Senior Lecturer
Department of Medical Oncology
Imperial College/Imperial Healthcare NHS Trust
Charing Cross Hospital
London
UK
გაფრთხილება:
JS declares that he has no competing interests.
William C. Dooley, MD
The G. Rainey Williams Professor of Surgical Oncology
University of Oklahoma
Oklahoma City
OK
გაფრთხილება:
WD declares that he has no competing interests.
რეცენზენტების განცხადებები
BMJ Best Practice-ის თემების განახლება სხვადასხვა პერიოდულობით ხდება მტკიცებულებებისა და რეკომენდაციების განვითარების შესაბამისად. ქვემოთ ჩამოთვლილმა რეცენზენტებმა თემის არსებობის მანძილზე კონტენტს ერთხელ მაინც გადახედეს.
გაფრთხილება
რეცენზენტების აფილიაციები და გაფრთხილებები მოცემულია გადახედვის მომენტისთვის.
წყაროები
ძირითადი სტატიები
World Health Organization. Mastitis: causes and management. 2000 [internet publication].სრული ტექსტი
Wilson E, Woodd SL, Benova L. Incidence of and risk factors for lactational mastitis: a systematic review. J Hum Lact. 2020 Nov;36(4):673-86.სრული ტექსტი აბსტრაქტი
Trop I, Dugas A, David J, et al. Breast abscesses: evidence-based algorithms for diagnosis, management, and follow-up. Radiographics. 2011 Oct;31(6):1683-99.სრული ტექსტი აბსტრაქტი
გამოყენებული სტატიები
ამ თემაში მოხსენიებული წყაროების სრული სია ხელმისაწვდომია მომხმარებლებისთვის, რომლებსაც აქვთ წვდომა BMJ Best Practice-ის ყველა ნაწილზე.
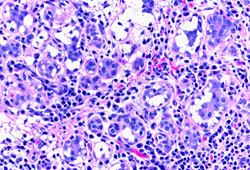
დიფერენციული დიაგნოზები
- Breast engorgement
- Nipple sensitivity
- Galactocele
მეტი დიფერენციული დიაგნოზებიგაიდლაინები
- ABM clinical protocol #36: the mastitis spectrum
- ABM clinical protocol #36: the mastitis spectrum
მეტი გაიდლაინებიპაციენტის ბროშურები
Mastitis in breastfeeding women
Mastitis: breastfeeding advice
მეტი პაციენტის ბროშურებიშედით სისტემაში ან გამოიწერეთ BMJ Best Practice
ამ მასალის გამოყენება ექვემდებარება ჩვენს განცხადებას