Summary
Definition
History and exam
Key diagnostic factors
- variable onset
- pink, red, or blue color
- rapid growth
- variable compressibility
- flat or nodular character
Other diagnostic factors
- islands of normal skin
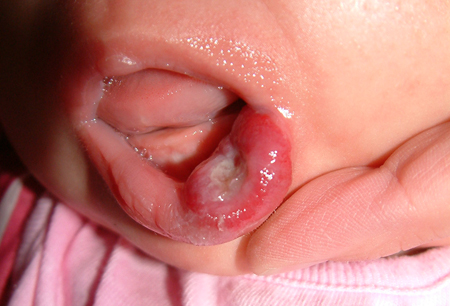
- ulceration and bleeding
- warmth
- history of low birth weight
- variable pain
- associated defects
- beard distribution and stridor
- lumbosacral location
- multiple lesions
- poor infantile feeding, failure to gain weight
- high-output cardiac failure
Risk factors
- low birth weight
- birth prematurity
- white ethnicity
- female sex
- maternal multiple gestation
- advanced maternal age
- chorionic villus sampling
Diagnostic investigations
1st investigations to order
- Doppler ultrasound of hemangioma
Investigations to consider
- MRI (without and with IV contrast) of hemangioma
- biopsy of lesion
Treatment algorithm
asymptomatic
with functional impairment or cosmetic disfigurement
Contributors
Authors
Kari L. Martin, MD
Associate Professor of Dermatology & Child Health
Pediatric Dermatology
University of Missouri – Columbia
Columbia
MO
Disclosures
KLM is an investigator in clinical trials with Scioderm, Lilly, and Durata; payments were received by her institution for these trials. None of these are relevant to this topic.
Acknowledgements
Dr Kari L. Martin would like to gratefully acknowledge Dr Tobian Muir, Dr Ingrid Polcari, Dr Annette Wagner, and Dr Carla T. Lee, the previous contributors to this topic.
Disclosures
TM, IP, and CTL declare that they have no competing interests. AW: none disclosed.
Peer reviewers
Elena Pope, MD
Head
Department of Dermatology
The Hospital for Sick Children
Toronto
Ontario
Canada
Disclosures
EP is an author of a number of references cited in this topic.
Elisabeth Higgins, MD
Consultant Dermatologist
King's College Hospital
London
UK
Disclosures
EH declares that she has no competing interests.
Iona Friedan, MD
Professor of Clinical Dermatology and Pediatrics
University of California San Francisco
San Francisco
CA
Disclosures
IF is a consultant for Pierre Fabre Dermatology, which is involved in clinical trials of propranolol for hemangiomas. IF is an author of a number of references cited in this topic.
Peer reviewer acknowledgements
BMJ Best Practice topics are updated on a rolling basis in line with developments in evidence and guidance. The peer reviewers listed here have reviewed the content at least once during the history of the topic.
Disclosures
Peer reviewer affiliations and disclosures pertain to the time of the review.
References
Key articles
Krowchuk DP, Frieden IJ, Mancini AJ, et al. Clinical practice guideline for the management of infantile hemangiomas. Pediatrics. 2019 Jan;143(1): e20183475.Full text Abstract
Darrow DH, Greene AK, Mancini AJ, et al. Diagnosis and management of infantile hemangioma. Pediatrics. 2015 Oct;136(4):e1060-104.Full text Abstract
Krowchuk DP, Frieden IJ, Mancini AJ, et al. Clinical practice guideline for the management of infantile hemangiomas. Pediatrics. 2019 Jan;143(1): e20183475.Full text Abstract
Reference articles
A full list of sources referenced in this topic is available to users with access to all of BMJ Best Practice.
Differentials
- Venous malformation
- Arteriovenous malformation
- Lymphatic malformation
More DifferentialsGuidelines
- ACR Appropriateness criteria for soft tissue vascular anomalies: vascular malformations and infantile vascular tumors (non-CNS)-child
- Vascular anomalies in childhood: When to treat and when to refer
More GuidelinesLog in or subscribe to access all of BMJ Best Practice
Use of this content is subject to our disclaimer