COVID, comorbidities, and evidence-based medicine
Author: Dr Kieran Walsh
Evidence-based medicine has been defined as “the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients.” (1) Evidence-based medicine is built upon original research, such as randomised controlled trials, and then on systematic reviews or meta-analyses of original research, with knowledge synthesis and translation into clinical guidance, guidelines and protocols Traditionally, all of these activities have taken years to carry out. It usually takes years to do the research, to appraise it, and to draw conclusions about how the evidence might be used in practice.
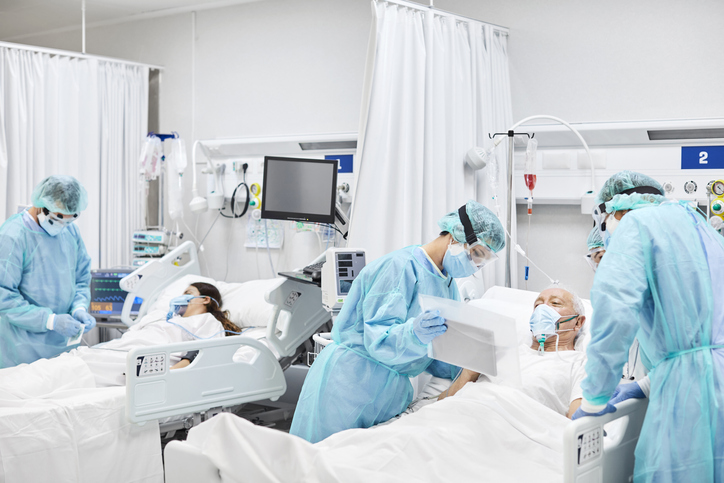
But the COVID pandemic has not given us years to make decisions – and as a result, some have questioned the role of evidence-based medicine in the pandemic. There are a number of reasons for this. Firstly when patients are critically ill as a result of a novel disease, it is tempting to think that the best thing to do is to give them any treatment that might help. This happened in the early months of the COVID pandemic. Certain treatments such as hydroxychloroquine were recommended without strong evidence of their effectiveness.
Secondly, in the midst of a pandemic, recommendations might be made without all relevant data being available. One example of this is research reports being press released without the full paper being published – which is not acceptable practice. Thirdly, in crisis situations, there can be an attitude of prescribing treatments that are unlikely to cause harm. However, there can be no guarantee of zero harm and thus it may be unwise to make treatment decisions on this basis alone. These issues existed before the COVID pandemic, but the pandemic has brought them to greater attention than ever before.
So how should evidence-based medicine evolve in light of these factors? It is worth going back to the core tenets of evidence-based medicine. These are the research base, patient needs and preferences, and professional expertise. The core tenet of professional expertise has become even more valued during the pandemic. Professionals are needed to assess patients and then to diagnose and treat the condition. The second core tenet is patients making decisions about their care. Patients clearly should be making decisions with their healthcare professionals about their care. The circumstances of the pandemic have made this more challenging than usual – but it is still a core principle of evidence-based medicine.
However, this still leaves us with problems with the evidence itself. Carley and colleagues provide some helpful suggestions in this regard. (2) They suggest that far more patients should be entered into trials – so that we can improve the evidence base; that trials should be of the highest possible quality; that we should make greater use of data that is available; and that certain trial protocols should be developed before pandemics so that they are ready to use when a pandemic occurs.
At BMJ Best Practice, we are working at the other end of the evidence pipeline – where evidence on COVID-19 and associated comorbidities is being put into practice. What we have learned is that accessing the evidence is almost as important as the evidence itself. This means content being available on a mobile phone, on an app, and integrated into electronic health records.
If there is more that we can do to support your evidence-based practice, please do let us know – we would be delighted to hear from you. Please email on kmwalsh@bmj.com.
References
1. Sackett DL. Evidence-based medicine. Semin Perinatol. 1997 Feb;21(1):3-5
2. Carley S, Horner D, Body R, Mackway-Jones K. Evidence-based medicine and COVID-19: what to believe and when to change. Emerg Med J. 2020 Sep;37(9):572-575.
Competing interests
KW works for BMJ Best Practice which produces evidence-based content on COVID-19.
